What's On This Page?
ToggleI feel like every family, including mine, somewhere in the ancestry has alcoholism and a person who wishes to be sober.
One of my close relatives has suffered with alcoholism and drug addiction since he was 14. Now, at over 60 years of age, he’s still suffering.
NOTE: Since the time of this writing in January 2017, things have taken a downturn. I was talking about my brother when I said “relative” above. He has sadly passed away. I couldn’t help him, I wish I could, I tried. You can read more in my other article, My Brother Was a Secret.
No One is Saying It Will Be Easy
The actual part of “quitting” is not as hard as staying sober thereafter. Most people who quit, start drinking again pretty soon after (or during) withdrawal. I hope to change that by educating you today. Whether it’s you or a close friend or family member who struggles with alcoholism or other drug addiction, one of my tips could very well change your life forever. I’m sure of it.
Once you start taking sedatives or drinking alcohol, you activate certain receptors in your brain that create the physical addiction in your body and then it becomes difficult to stop. After 3 weeks of routine use, it’s no longer easy to stop. You’re hooked.
I used to work in addiction and rehab centers in Central Florida. I’d also see alcoholics and addicts in the hospital. Alcoholism recovery is difficult, and the withdrawal phase is downright awful. I mean A.W.F.U.L! I bet some of you want to die when you’re in the middle of withdrawal, but I’m telling you that if you choose to hold on and prove your courage, YOU WILL be well. I promise you.
Whatever the day is, or time of year you can do it. Even if it’s around New Year’s when people often feel like it’s a good time to quit drinking, you should just do it. At least TRY.
Even if you have fallen off the wagon, try again. There’s a reason why people have trouble staying sober, or quitting their pot, or their sedatives… whatever it is, maybe I can lend some wisdom.
I’ve classified the sedative/hypnotics and benzodiazepine drugs along with alcohol because they impact similar receptors and brain chemicals. Speaking of benzodiazepines, they’re okay if you take them for a couple of weeks, or less, and in very low doses. If you have been on them awhile, you may want to take a look at THIS ARTICLE to learnmore.
I want to get you well.
I love receiving your emails with your positive stories, which you can email to: scriptessentials@gmail.com
If I can help YOU, it will positively affect your entire family. You may feel like your relationships are broken forever due to your past behavior and moods, but most relationships are mendable in time if both parties want to mend it. Your family and friends still love you, even if they are hurt by your behavior. They need you to get well and stop this nonsense. If you want to be helped and get sober once and for all, here are some tips:
1. To Recover from Alcoholism Develop Patience
This is #1 on my list because it’s the most important. Failure occurs when people give up instead of bearing with it, and holding on. Those receptors in your brain can and do heal. You see, if you drink or take benzodiazepine sedatives, the GABA receptors on your cells are atrophied. This means the little areas on your cells that hug GABA and pull it into your cell are essentially dead. It’s called “downregulation.”
Time is the only thing that will allow those receptors to regrow and heal. This is why you have to be patient and have faith. The receptor sites will upregulate. When they do, the awful symptoms of withdrawal, which may include anxiety, restlessness, gloom, insomnia, internal buzzing, cravings, torture in your brain and akathisias, will lessen. There are other symptoms that go hand in hand with GABA receptor downregulation, I’ve only mentioned a few. It could take up to two years for you to feel well, but you must hold on. You can do it.
2. How Supplements Might Backfire
Your brain has about one hundred billion neurons (cells) and there is a small space between them. The neurons don’t touch. The space between them is called a synapse. That’s where your “happy” brain chemicals hang around. The chemistry of addiction and staying sober is such that all these feel-good endorphins are needed constantly.
So when you suddenly stop receiving your endorphins (in the form of alcohol, antidepressants, benzodiazepines, or opiates like hydrocodone or heroin), your synapses starve. The “happy” brain chemicals aren’t there anymore. This is how cravings set in. This is in part why drug-seeking behavior occurs and why depression can be so profound if you don’t taper slowly enough.
Conventional medicine’s answer to this is to prescribe medications quickly… because they restore some feel-good endorphins. So physicians who are not knowledgeable in addiction and withdrawal will then increase neurotransmitters by prescribing a drug for it.
They are trying to push the production of a neurotransmitter, but if it’s done prematurely, you will suffer. I’ll explain why: if your receptors are downregulated, the new medication will backfire since there’s no receptor to hug it in. You have taken a medication or supplement to ease withdrawal, yet you feel worse on it.
The key is to re-sensitize your receptors, not push production of endorphins… there’s nowhere for them to go, their levels spike in the space (the synapse) and build up, causing terrible side effects. I’m not completely against supplements (or medications for that matter), but I feel like timing and proper dosage is everything.
3. Microdose Test Supplements
There are dozens of options that have the possibility to help you raise GABA, but if you keep in mind what I just taught you above, then it’s obvious you need to begin with microdoses.
Let’s use our example of alcohol, which mimics GABA’s function in the body in that it’s calming. Supplements that may help raise GABA include lemon balm, magnolia bark, passionflower, valerian root and more. I don’t recommend any of them early on, but maybe after a few months of sobriety.
This is highly individual, so please don’t take my word as gospel. But whatever you and your doctor decide, microdosing is key to using any of those supplements and others not listed here.
The point is this: you make GABA in your body out of the precursor amino acid called glutamate. When glutamate builds up you feel anxiety, internal restlessness, panic, pain and possibly digestive problems, especially in your pancreas. You need to make sure that conversion of glutamate into GABA is happening properly.
This is a huge tip for people trying to stay sober, so please remember it. The conversion of glutamate into GABA is what keeps you calm and helps to reduce cravings. It’s not the actual level of glutamate or GABA, it’s how efficiently you convert glutamate into GABA. You need both of those, neither is a bad guy.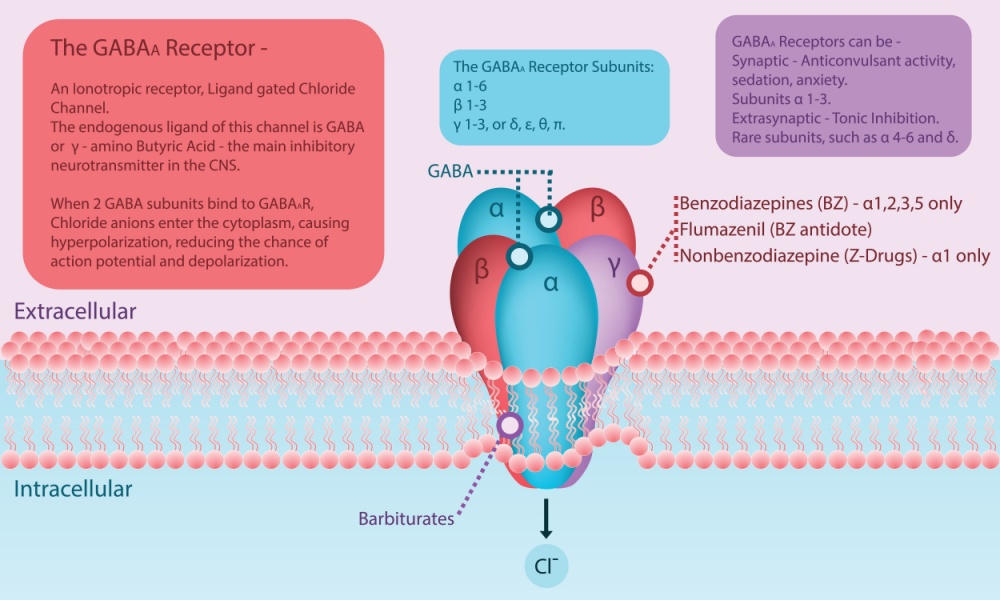
Converting glutamate into calming GABA requires an enzyme called GAD (glutamate decarboxylase) which is generated in your pancreas. What if you don’t make enough GAD? Many people with alcoholism don’t have enough, that’s why it’s hard to stay sober.
What if you have a genetic SNP against this enzyme, or antibodies against this enzyme? It’s going to spark a lot of intestinal disturbances that will confuse you and probably your gastroenterologist (because nothing shows up but you hurt like heck).
GABAa and Alcoholism
Alcohol primarily impacts the GABA-a (Gamma-Aminobutyric Acid type A) receptors in the brain. These receptors are part of a class of receptors known as ligand-gated ion channels. GABA is the main inhibitory neurotransmitter in the brain, and its role is to reduce neuronal excitability throughout the nervous system.
When alcohol binds to GABA-a receptors, it enhances the inhibitory effects of GABA by increasing the flow of chloride ions into the neuron. A complicated way to say it is calming! And we know alcohol can be calming for some people, but not all! Definitely not all people, some it is just the opposite.
Anyway, this binding action initally results in an inhibitory effect on the central nervous system (CNS) leading to the sedative, anxiolytic (anxiety-reducing), and at times, the impairing effects associated with alcohol consumption.
Visceral Hypersensitivity
This is called “visceral hypersensitivity” and it’s quite common in alcoholics and those recovering from benzo and opiate misuse and abuse. This is why I told you that you might have digestive problems, either in the middle or side of your abdomen. Glutamate builds up in the nerves surrounding your digestive organs, especially your pancreas which creates GAD and if GAD is not working well, glutamate builds up. Remember, glutamate is painful in excess.
This next piece is very important in order for you to get well. Your GAD enzyme doesn’t work well without several natural nutrients including P5P (pyridoxal 5 phosphate) the biologically active form of B6.
This P5P can be purchased online. Don’t depend on your body to convert the B6 to P5P, it isn’t going to happen. Also, don’t buy anything I mention without first asking your doctor, as I don’t know what’s right for you individually. I write to millions of you at once. So please, check to be sure if something I mention is right for you before you drive over to the health food store or buy online.
Now, you may be inclined to take 20 or 30 milligrams of P5P but I’m warning you, this will probably end badly. Microdoses along the lines of 5 or 8 mg taken two or three times a day is much better because this keeps GABA production steady and slow (remember, your GABA receptors are downregulated).
Just dump out the capsules in the sink and guesstimate a dose. This is not a cure for alcoholism, nor will it keep a person sober, it’s just to restore nutrients which cut down on some ‘side effects’ of drinking.
Lysine is also needed in order for P5P to work well. The two together help support GAD enzyme which then functions as the catalyst to turn glutamate into GABA. Probiotics can be helpful as well, but do not introduce all three supplements at once.
4. Build a Support System to Stay Sober
If you deal with alcoholism, find a great support network that includes professionals. There are many qualified, experienced, caring physicians and addiction/withdrawal counselors available. Social workers are also in a unique position to help you achieve sobriety.
Having the “help” of a physician untrained in addiction can set you back at the least, and at the worst be catastrophic for your recovery.

I’ll have more on this topic again soon. I think millions of people worldwide can benefit. Excessive drinking numbs you from the pain of past abuse or current emotional or physical trauma or stress. It’s an outlet for some, a way to decompress. It usually starts innocently with a glass or two of wine with dinner, and then slowly, alcohol takes over your life.
I know functional alcoholics. They are just like normal, and professionally successful, some are open about their drinking, others keep it a secret due to fear of judgment. Wherever you are in this, I hope today’s tips are useful.
I hope I’ve given you some insight today, as well as faith to be patient and know there’s a light at the end of the tunnel. Hang on please, because in time you will be well. It might be hard to see this right now but you can do it.
I’m rooting for you!
Related Articles:
How to curb cravings for alcohol and drugs
Milk thistle can liven up your liver
Akathisias make you want to jump out of your skin

Suzy Cohen, has been a licensed pharmacist for over 30 years and believes the best approach to chronic illness is a combination of natural medicine and conventional. She founded her own dietary supplement company specializing in custom-formulas, some of which have patents. With a special focus on functional medicine, thyroid health and drug nutrient depletion, Suzy is the author of several related books including Thyroid Healthy, Drug Muggers, Diabetes Without Drugs, and a nationally syndicated column.
