What's On This Page?
ToggleEvery so often someone tells me a story that begins like this:
“My heart suddenly started racing. It felt irregular, like it was skipping around. I thought it was anxiety… but something didn’t feel right.”
I’ve heard that exact sentence more times than I can count. Sometimes it is anxiety. But sometimes it’s atrial fibrillation, commonly called AFib.
It’s actually very common. Its prevalence increases sharply with age, and studies estimate that more than 4% of people over age 60 have it. But once you understand what’s happening – and why doctors treat it the way they do – it becomes far less mysterious.
Let’s walk through it clearly.
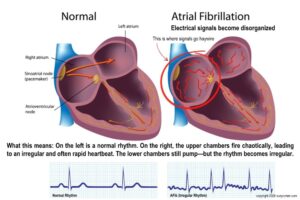 What Atrial Fibrillation Actually Is
What Atrial Fibrillation Actually Is
Your heart normally beats in a coordinated rhythm because electrical signals travel through it in an organized pattern.
In atrial fibrillation, the electrical activity in the upper chambers of the heart (the atria) becomes chaotic. Instead of contracting normally, the atria quiver or fibrillate. This causes two things to happen:
- The heartbeat becomes irregular
- The heart rate may also become very fast
Instead of a steady rhythm, the pulse becomes what cardiologists describe as “irregularly irregular.” Some people experience episodes that come and go. It’s called paroxysmal AFib, which simply means the rhythm typically stops on its own within seven days.
What AFib Feels Like
These are the most common symptoms reported:
• rapid or pounding heartbeat
• fluttering sensation in the chest
• shortness of breath
• dizziness or lightheadedness
• fatigue or weakness
• reduced exercise tolerance
Many people describe the sensation as though “a fish was flopping in my chest.”
In some cases, the heart rate may rise to 160–180 beats per minute, which is often what brings people to the emergency room. Interestingly, research shows many AFib episodes are silent, meaning they occur without any symptoms! This is why some people discover the condition only during a routine exam or after a smartwatch alerts them to an irregular pulse.
When Should You Seek Medical Care?
If you experience a sudden irregular heartbeat, it’s worth being evaluated.
Seek emergency care if you experience any of this:
• a very rapid heart rate
• chest pain
• shortness of breath
• fainting or near-fainting
• severe dizziness
Even if symptoms improve, a first episode of AFib should be evaluated by a healthcare professional. The reason is simple: AFib isn’t just about symptoms. It’s about stroke risk.
AFib Can Lead to Stroke
The biggest concern with AFib is blood clots. When the atria are quivering instead of contracting normally, blood can pool in a small pouch of the heart called the left atrial appendage. When blood sits still, it can form a clot.
If that clot travels to the brain, it can block an artery and cause a stroke.
What Happens in the Emergency Room
When someone arrives in the ER with AFib and a rapid heart rate, the first priority is often rate control. In other words, doctors try to bring the number of beats per minute down to a safer level.
Doctors commonly use medications such as diltiazem or metoprolol, two well-established drugs that slow conduction through the heart’s atrioventricular (AV) node. These medications are often given intravenously (IV) in the emergency setting because they work quickly, sometimes within minutes.
But the important point is that they don’t necessarily stop the AFib itself. Instead, they slow the pulse from something like 170–180 beats per minute down to a safer range, often around 90–110 beats per minute. This helps stabilize the patient and reduce symptoms such as dizziness, shortness of breath, or chest discomfort.
Once the heart rate is controlled and you’re stable, the ER doctor will decide whether to:
• allow your heart rhythm to convert naturally, which it often does in cases of paroxysmal AFib (sometimes within a few hours or within the first day)
• use medications to restore normal rhythm, such as antiarrhythmic drugs like amiodarone, flecainide, or propafenone, depending on the patient’s situation
• perform electrical cardioversion, a brief procedure that delivers a controlled electrical shock to restore normal rhythm
Many patients with paroxysmal AFib can go home the same day with follow-up care arranged, especially if their symptoms improve and their stroke risk has been assessed. In plain English, they’re trying to slow things down so you feel better and stay safe. A landmark study called the AFFIRM trial found that controlling heart rate can be just as effective as trying to force the heart back into a normal rhythm for many patients.
Why Doctors Prescribe Oral Anticoagulants
Blood thinners reduce the chance that a clot will form and travel to the brain. The most common oral anticoagulants today include:
• ELIQUIS (apixaban)
• Xarelto (rivaroxaban)
• Pradaxa (dabigatran)
• Coumadin (warfarin) –> this one has fallen out of favor due to difficulty in monitoring it, its ability to cause excessive bleeding, and dietary restrictions.
A landmark clinical trial called the ARISTOTLE STUDY found that apixaban reduced stroke and major bleeding compared with warfarin in patients with atrial fibrillation.
These medications do not dissolve existing clots. Instead, they reduce the blood’s tendency to form dangerous ones.
Understanding the CHA₂DS₂-VASc Score
Doctors use a risk assessment tool called the CHA₂DS₂-VASc score to estimate stroke risk. When spoken aloud, it’s usually pronounced “chad-vask.” Here’s a graphic I made for you so you can calculate your own score. I think it will offer insight into why some people are treated more aggressively with blood-thinners while others are not. This scoring system is widely used in cardiology guidelines to determine who should take blood thinners.
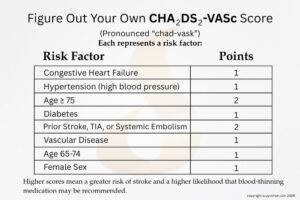

General guideline thresholds (ACC/AHA/ESC)
Take the test now, see what your score is:
For men
-
0 points → anticoagulation usually not recommended
-
1 point → anticoagulation may be considered
-
≥2 points → anticoagulation recommended
For women
-
1 point (female sex only) → no anticoagulation
-
≥2 points → anticoagulation usually recommended
In many cases, people with a chad-vask score of 0 (for men) or 1 due only to female sex for example, are considered low risk for stroke and wouldn’t necessarily need lifelong treatment with blood thinners. But still, some doctors sometimes prescribe a short course of an anticoagulant after a new AFib episode for a few reasons. And you might wonder why if their score is zero or one. First of all, the atria may remain temporarily “stunned” after an AFib episode, which can briefly increase the chance of clot formation while the heart rhythm stabilizes.
Here’s where this gets a little nuanced.
If the rhythm was restored using cardioversion (either with medication or an electrical shock), cardiology guidelines do recommend anticoagulation meds for several weeks afterward – it’s just as a precaution. It will almost always be discontinued after a few weeks (but obviously ask your doctor). Doctors may not know exactly how long the AFib episode was going on before it was detected so that’s another reason.
Like, did you sit there with it for six, eight or even 12 hours before going to the emergency room… or did you go within minutes of it starting. If it may have lasted more than a day or two, a short course of anticoagulation is sometimes used to reduce clot risk during that period.
In people with low “chad vask” scores, this treatment is often temporary rather than lifelong, and the decision is usually reassessed at follow-up.
Cautions About Aspirin and Fish Oil Supplements
Eliquis and others in this category are expensive drugs, so you may be wondering if you can just take cheap aspirin instead. It’s a valid thought, however, I don’t think so. You see, years ago, aspirin was actually used for stroke prevention in AFib, and it was pretty common. But today we know that aspirin provides far less protection than anticoagulant medications.
So today, most current cardiologists no longer recommend aspirin alone for stroke prevention in atrial fibrillation. They use one of the oral anticoagulants listed above. The most affordable one if you pay cash is the warfarin.
Fish oil supplements are widely used for heart health, and at times even recommended by the American Heart Association, but the relationship with AFib is complex. I want you to have all the information about this.
Omega-3 fatty acids such as EPA and DHA (fish oils) can lower triglycerides and help with inflammation. We also know they positively impact blood clotting pathways. But they’re not always good for you. Several large studies suggest high-dose fish oils may increase the risk of AFib in some folks. In fact, large trials such as the STRENGTH study observed a slightly higher incidence of AFib in people taking very high doses of omega-3 supplements. Surprised? I was!
This doesn’t mean fish consumption or fish oil supplements are harmful. But high-dose fish oil capsules are not an actual treatment for AFib.
When I say “high-dose fish oil,” I’m talking about 3,000 mg or more per day of combined EPA and DHA, and especially that 4,000 mg (4 grams) daily range. Like, that’s the big one used in prescription products like VASCEPA and in clinical trials for lowering very high triglycerides. It’s not your typical “one capsule a day” situation. And here’s the nuance that surprised even me: At these higher levels, several large well-designed studies proved a small but real increase in the risk of atrial fibrillation!
Less is more when it comes to this supplement and heart rhythm.
Common Triggers and Risk Factors
AFib often develops when the heart’s structure or electrical system changes. The most common risk factors are:
• aging
• high blood pressure
• sleep apnea
• obesity
• coronary artery disease
• thyroid disorders (Hyperthyroidism or GRAVES’ is the thyroid disorder most strongly associated with atrial fibrillation. Here are the 10 KEY SYMPTOMS)
• alcohol use (Did you know drinking alcohol leads to insomnia? Here’s HOW)
• diabetes
Structural heart problems such as enlarged heart chambers or certain valve diseases, can also contribute.
Many people assume AFib appears “out of nowhere,” but cardiologists often see patterns behind episodes. Several common triggers can irritate the heart’s electrical system or make it easier for abnormal rhythms to start. Some of the most frequent include:
• Sleep apnea – One of the strongest and most underdiagnosed contributors to AFib. Interrupted breathing during sleep stresses the heart and raises blood pressure overnight.
• Alcohol (“holiday heart”) – Even moderate alcohol intake can trigger AFib episodes in susceptible individuals.
• Thyroid imbalance – An overactive thyroid can make the heart more electrically unstable.
• Electrolyte disturbances – Low magnesium, potassium, or dehydration can make heart cells more excitable.
• High stress or excess adrenaline – Surges of sympathetic nervous system activity can precipitate episodes.
• Illness or infection – Fever, inflammation, and systemic stress can temporarily trigger arrhythmias.
• Structural heart changes – Enlargement of the left atrium, high blood pressure, or long-standing valve disease can create an environment where AFib is more likely.
Researchers also believe premature atrial beats (PACs)—small early electrical impulses that often arise near the pulmonary veins—may act as triggers for AFib episodes in susceptible hearts. Addressing triggers can sometimes reduce the frequency of episodes.
Can Wearable Devices Detect AFib?
Smartwatches and wearable heart monitors have become increasingly useful. Devices such as the Apple Watch can detect an irregular pulse pattern and alert users. These devices are not perfect, but they can help identify abnormal rhythms earlier and prompt medical evaluation. Still, a formal diagnosis requires electrocardiography (ECG) or clinical monitoring. A study called VITAL-AF showed that simple ECG screening during routine visits can uncover previously undiagnosed AFib.
Why Sleep Apnea and Alcohol Matter More Than Most People Realize
Two factors repeatedly show up in cardiology clinics when patients develop AFib. It’s sometimes sleep apnea and sometimes alcohol. Let’s talk about apnea first.
Sleep apnea
In obstructive sleep apnea, breathing repeatedly stops during sleep. This leads to drops in oxygen, a surge in cortisol (a stress hormone), and a sudden blood pressure spike. Over time, this nightly stress can enlarge the left atrium and disrupt electrical stability. Studies consistently show that treating sleep apnea article can reduce AFib recurrence, especially after cardioversion or ablation procedures.
If someone you love snores loudly next to you, always wakes up tired, or has pauses in breathing during sleep that you can hear, I think it’s worth getting a sleep study.
You can do these sleep studies from your own home now. You don’t have to go to a sleep clinic and get all hooked up in wires and sleep in an unfamiliar bed! A lot of people don’t realize that, and therefore never get a sleep apnea study. Because sleep apnea plays such an important role in heart rhythm disorders, it’s worth understanding the different types. You can learn more in my companion article: Understanding the Difference Between Central Sleep Apnea and Obstructive Sleep Apnea.
Alcohol (“holiday heart”)
Drinking too much alcohol has a well-known connection to AFib. Even in people with otherwise healthy hearts, episodes can occur after heavy drinking (or binge), or after a holiday celebration where a lot of alcohol is served. This phenomenon is sometimes called holiday heart syndrome.
Alcohol can damage the body in so many ways due to oxidative damage. It can irritate heart cells, alter the balance of your electrolytes and increase adrenaline – all of which are bad for AFib. For people who are prone to AFib, reducing or eliminating alcohol lowers the chance of recurrent episodes. Alcohol can also interfere with sleep in ways many people don’t realize. If you’d like to understand why a nightcap often leads to restless sleep later in the night, read my article: 8 Surprising Reasons that Alcohol Causes Insomnia.
Supporting Heart Rhythm: Nutrients and Lifestyle Strategies
While medications and medical evaluation remain essential, some lifestyle and nutritional factors may support overall heart rhythm stability.
It’s important to remember that supplements do not replace medical care, but certain nutrients are commonly discussed in the context of heart rhythm health.
Some examples include:
Magnesium
Magnesium plays a key role in electrical signaling in heart cells.
Low magnesium levels can contribute to:
• palpitations
• premature beats
• rhythm instability
Many cardiologists monitor magnesium in patients with arrhythmias, and maintaining healthy levels may help support normal rhythm.
Coenzyme Q10 (Ubiquinol)
CoQ10 helps support mitochondrial energy production in heart muscle.
The heart is one of the most energy-demanding organs in the body, and adequate cellular energy may help maintain normal cardiac function.
Taurine
Taurine is an amino acid involved in:
• electrolyte balance
• calcium signaling in heart cells
• stabilization of cardiac electrical activity
Some research suggests taurine may help support normal rhythm in certain individuals, though more large clinical studies are needed.
Electrolytes and hydration
Adequate hydration and balanced electrolytes are often overlooked, but it doesn’t take much to fall out of balance. Sometimes you forget to drink during the day, or you have coffee (which has a mild diuretic effect). This situation can alter levels of sodium, potassium and magnesium which becomes a problem, and increases risk for AFib. All of these influence electrical activity in the heart. Maintaining good hydration and electrolyte balance can be especially important during illness, heat exposure, or intense exercise.
Omega-3 fatty acids
High-dose fish oil supplements have shown mixed effects in AFib research.
⚠️ Large clinical trials suggest that very high doses of omega-3s can slightly increase AFib risk in some people, so supplementation should be individualized and discussed with a physician.
The Big Picture
AFib is rarely caused by just one factor. Here’s what I think are the most common combinations that trigger an episode:
• Electrical triggers – Sometimes stray electrical signals in the heart fire at the wrong time and start the irregular rhythm seen in AFib.
• Structural heart changes – When the heart becomes enlarged, stiff, or damaged over time, its electrical system can become less stable.
• Metabolic stressors – Illness, hormone problems, inflammation, or low minerals like magnesium or potassium can stress the heart and disturb its rhythm.
• Lifestyle factors – Things like alcohol, poor sleep, dehydration, or high stress can sometimes trigger an episode of AFib.
For many people, the most effective approach involves both medical care and addressing underlying contributors such as sleep apnea, blood pressure, alcohol intake, and electrolyte balance. That combination can go a long way toward helping the heart maintain a stable rhythm.
Questions to Ask Your Doctor if You Have AFib
If you’ve been diagnosed with atrial fibrillation—or think you may have it—it’s helpful to go into your appointment with a few key questions. These can help you understand your personal risk and make informed decisions about treatment.
Here are some good questions to start with:
• What type of AFib do I have?
(AFib can be paroxysmal, persistent, or permanent, and treatment may differ.)
• What is my CHA₂DS₂-VASc score?
This score estimates your stroke risk and helps determine whether you should take a blood thinner.
• Do I need an anticoagulant medication to prevent stroke?
If so, ask about the benefits, risks, and which medication may be best for you.
• Should we focus on controlling my heart rate or restoring a normal rhythm?
Some people do well with rate control alone, while others benefit from rhythm treatments.
• Could sleep apnea be contributing to my AFib?
Sleep apnea is a common but often overlooked trigger for atrial fibrillation.
• Should I be tested for thyroid problems or electrolyte imbalances?
Hormone issues and low minerals such as magnesium or potassium can sometimes affect heart rhythm.
• Would a heart monitor or wearable device help track my episodes?
Short-term monitors or wearable technology can help detect intermittent AFib.
• What lifestyle changes might help reduce episodes?
Ask about alcohol, caffeine, sleep habits, hydration, and stress.
• When should I seek emergency care if symptoms return?
Knowing this ahead of time can help you respond quickly if another episode occurs.
The more you understand your condition, the easier it becomes to work with your doctor on a treatment plan that protects your heart and lowers your stroke risk.
The Bottom Line
Atrial fibrillation can feel alarming when it first occurs, but it is a common and manageable condition. This is critical for you to know:
• you need to seek medical care when appropriate
• understanding your stroke risk can save your life
• following medical advice about anticoagulation if recommended
Most importantly, AFib treatment isn’t just about controlling a racing heart. It’s about protecting your brain from stroke. With proper evaluation and the right treatment plan, many people with AFib live full, active lives. Once you understand what’s happening, it becomes a lot less scary.

Suzy Cohen, has been a licensed pharmacist for over 30 years and believes the best approach to chronic illness is a combination of natural medicine and conventional. She founded her own dietary supplement company specializing in custom-formulas, some of which have patents. With a special focus on functional medicine, thyroid health and drug nutrient depletion, Suzy is the author of several related books including Thyroid Healthy, Drug Muggers, Diabetes Without Drugs, and a nationally syndicated column.


