What's On This Page?
ToggleI made a commitment to dive into your inquiries, and true to my word, this blog post is all about shedding light on those. Today, we’re tackling the insightful questions you sent my way about thyroid dysfunction, peroxide treatments, and Hashimoto’s, following our recent newsletter discussion.
Firstly, wow—your curiosity and intelligence shine through every question! Selecting which ones to address here was no small feat, given the depth and quality of your submissions. I noticed a recurring theme in your questions, so I’ve chosen those that I believe will resonate with most and provide substantial insight.
I’ve dedicated considerable time to research and have included links to my other videos, books, and articles to deepen your understanding. If you’re still curious or have further questions, feel free to use the search box located at the top right corner of this page—I’ve got a treasure trove of over 1,000 exclusive articles waiting for you. Plus, for those who prefer visual content, don’t forget to check out my YouTube channel for more guidance.
As we dive into the responses below, please remember that while I aim to inform and support, I’m not a medical professional. It’s crucial to consult with your healthcare provider to tailor any information to your specific health needs. I’m here to share knowledge and perspectives, not to replace professional medical advice. Thank you to everyone who contributed questions. Let’s get started!
Gray Hair and Vitiligo
Question
Is systemic Hydrogen Peroxide the cause of gray hair and vitiligo? Thanks.
Chris
Answer: Yes, it’s not the cause of everyone’s grey hair but it contributes. Remember, peroxide (in excess) is an oxidizer. Let me speak to the vitiligo part since this is a frustrating autoimmune condition that doesn’t have a lot of treatment options: Hydrogen peroxide blocks normal production of melanin, and the vitiligosupport.org site even mentions “hydrogen peroxide” on the home page. There are even catalase-based creams that you can apply to the skin to reduce epidermal levels of peroxide allowing for noticeable repigmentation. Taking catalase internally maybe even more helpful. I read an article that concluded the “necessity necessity of epidermal H2O2 removal … in the successful treatment of vitiligo.”
Borderline Thyroiditis
Question:
Dear Suzy,
After suffering for over 15 years with borderline thyroiditis I finally succumbed to trying thyroid medication. Taking the medication or not taking it, raising it, lowering it – I still feel the same, constantly fatigued, achy, sluggish, foggy thinking, headaches and dizzy with perfect blood work of course! Is there help for people like me? Thanks so much for all you do.
JoAnn G.
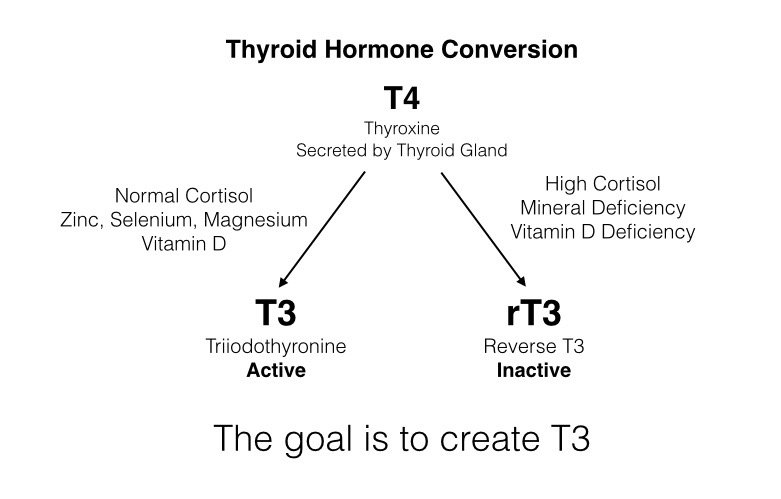
Answer: Hi JoAnn– Yes there is HELP. One of the questions I would ask is what type of “thyroid medication” did you take? For example, if it was a T4 drug (like Levothyroxine), then perhaps it was not converting in your cells to the biologically active form of T3. Many things block T4 to T3 conversion, and I have excerpted a chart that is in my thyroid book which you can see on the right.
Blockers of T4 to T3 Conversion
Among the things that block conversion:
High Cortisol
Deficiencies in minerals like selenium, zinc or magnesium
Low vitamin D
So if you take a T4 drug and have these problems all your T4 medication will convert to rT3 (reverse T3) which makes you hypothyroid, and you’ll feel awful.
Also, if you have adrenal burnout, then that has to be fixed first, and you’ll need adrenal adaptogens and rest, before you even attempt to take more thyroid medicine.
A combination of T4 with T3, or a pure T3 drug might be in order, but first fix those adrenals if they are worn out from work, stress and/or illness.
Most of all, do not give up hope! There is more about this in my Thyroid Healthy book.
Typical Hashimoto’s Patient wi
th Exhaustion
Question:
Hi Suzy!
Thank you for all the information you put out to help your readers and loyal followers. I am probably your typical Hashimoto’s patient. I struggle with my labs being normal but my TSH, T4, and T3 are all at the very lowest end of the their ranges and I’m extremely exhausted and overweight. I currently see a functional medicine doctor and despite medication and going gluten, dairy, and soy free I’m still not “well.” I’ve been taking supplements like selenium, vitamin D3, zinc and magnesium along several others and the fatigue is relentless. What am I missing here? Thank you for all your help.
Danielle
Answer: Hi Danielle– Something is definitely missing because with all that you should be feeling better. If you don’t have a copy of my book already, Thyroid Healthy please consider it. I have a chapter on adrenal dysfunction as it pertains to the thyroid gland. This could be the missing piece. As long as your adrenals are weak, the thyroid won’t heal. Also, there may be an immune problem that is yet undetected. Please watch this on YouTube, I posted it for free to help people just like you. It has a lot of information on thyroid.
I recommend you do autoimmune testing through Cyrex Labs. Your mitochondria are beat up, stay in touch with me through my newsletter, as I plan to do more articles on reviving those energy generators. And finally, infections and mold are certainly possibilities that cause long-standing chronic intractable fatigue. I wish you the best.

_____
Question:
Suzy, You are a life saver. Finally someone who understands. I have been swinging back in forth from Dr. to Dr. for years, and have been told to “wait and see” too many times.
Recently my new endocrinologist sent me back to my primary care doctor because he couldn’t do anything else for me. The same primary care doctor who sent me to him because she didn’t know how to treat Hashimoto’s.
She told me it was my hormones and sent me to gynecologist who wanted to start me on HRT and antidepressants. I am not depressed, I am frustrated. I just want to feel like my old self again.
My question is, should I keep looking into the hormone issue, or just address the Thyroid. I am running out of options and money. Thank you for your help,
Cheryl
Answer: The problem is that physicians only know how to use tools that are in their own tool box so if you don’t fit what they typically treat, you are referred out. It’s insulting to assume that it’s your hormones when they didn’t test you through Rhein or Dutch. It’s an assumption, along with the “depression” diagnosis which is almost always assumed. Hormones are fine to test, but if money is tight, I’d pass for now. Correcting estrogen, progesterone, testosterone, DHEA and the rest STILL won’t stop the autoimmune attack you’re experiencing.
So put your money into the following tests through Cyrex. These 3 tests will help you determine which foods are driving your Hashimoto’s, and going off them should calm the storm so do: Cyrex Array 3, Cyrex Array 4, Cyrex Array 10. In the meantime, I highly recommend you eliminate gluten and dairy, and possibly eggs if you can. I’d also continue to address your thyroid and make sure you have recent levels of TgAb and TPOAb. Keep an eye out for my videos that discuss hydrogen peroxide too, reducing that is crucial.
Radioactive Iodine for Graves’ Disease
Question:
Suzy,
I was treated with radioactive iodine (twice) almost twenty years ago for Graves’ Disease, and am on 137 mag of Synthroid, that’s my only prescription. I would be interested in knowing what blood tests to do, and how to adjust as naturally as possible. Especially concerned with how Graves’ effects eyes. I really appreciate the effort that you’ve all put into the Functional Medicine webinars!
Lynda
Answer: Hi Lynda. Synthroid (levothyroxine) is a T4 drug and in order for it to become biologically active and work as true thyroid hormone, you have to convert it in your body to another compound called T3. You may want to take a moment to read my other article, How Stress and Cortisol Impact Hashimoto’s and Graves’ Disease.
That’s a natural process that healthy people can do, however if you have been sick a long time, or you have lots of inflammatory compounds in your body, T4 drugs don’t work well. You cannot convert them to T3 so I’m worried that you are taking a medication that doesn’t work. I would ask doc about taking some pure T3 medications instead. Two tests I would ask your doctor for include:
TBII (Thyrotropin binding inhibiting immunoglobulins)
TSH receptor antibodies
If you could do more tests, I highly recommend: Cyrex Array 4 and 5 which will test you for food sensitivities as well as multiple other autoimmune problems.
As for natural solutions to something like Graves’ ophthalmopathy (eye symptoms), there are some options. First, let me list a few symptoms for the benefit of others reading this so they know what Graves’ ophthalmopathy:
Bulging (exophthalmos)
Dryness or redness
Eyelid lag
Eyelid retraction
Blurry vision
Tearing
Feeling of grittiness or foreign body
Double vision (diplopia)
Staring appearance
You may be interested in learning about 3 Advantages of Tepezza for Thyroid Eye Disease.
These symptoms may respond to selenium, vitamin E, vitamin D and possibly Riboflavin (B2). Bugleweed is an herb that helps with Graves’ disease and the eye symptoms. Also, medication such as Low Dose Naltrexone (LDN) would be an option, I have started recommending really low doses of this, for example 1.0 or 1.5 mg at night, not 4.5 like many recommend. I’ve heard too many problems like bad dreams and insomnia occurring with that dose, so again LDN 1.0 or 1.5 mg (milligrams) at night if tolerated. Dreams and nightmares may prevent this type of dose but most people do well.
Question:
Hi Suzy and thank you so much for your work!
My doc says I have a “sluggish thyroid.” My lab results are all within range so she’s going by symptoms, mainly my complete inability to lose weight no matter what and low waking temperature among a few other things associated with thyroid, but says I do not have Hashimoto’s based on the antibody tests: TPO Ab = 11 IU/ml and my Tg Ab = <1.0 IU/ml [Reference range 0.0-0.9]
I’ve read it’s possible to have autoimmune thyroid disease with no antibodies and you say the same as most: most hypoT is hashi’s.
What is the way I can get a definitive answer on whether or not I have hashi’s? I already have a diagnosis of alopecia areata concurrent with vitiligo and I’ve also read that having AI conditions may increase my chances of developing other AIs.I’ve been gluten-free for >2 years and eat a modified paleo diet. Thank you!!!
Cynthia
Answer: Hi Cynthia. Yes, it’s possible to have autoimmune thyroid disease even though your antibodies are close to normal. I would say though, that at 11, that is actually positive. New research suggests that the range for these antibodies should be something like 9 or less. So 11 is just above that so in my opinion, you are showing high enough antibodies to qualify for the condition, but it’s also based upon your clinical signs and symptoms.
Sometimes the body doesn’t mount a full immune response so the labs come back messed up. You already have two different autoimmune disorders, the alopecia aerate and the vitiligo. The vitiligo is sometimes associated with deficiencies in the enzyme Catalase, which I talked about in Video 2. Both my videos are now archived on this page by CLICKING HERE.
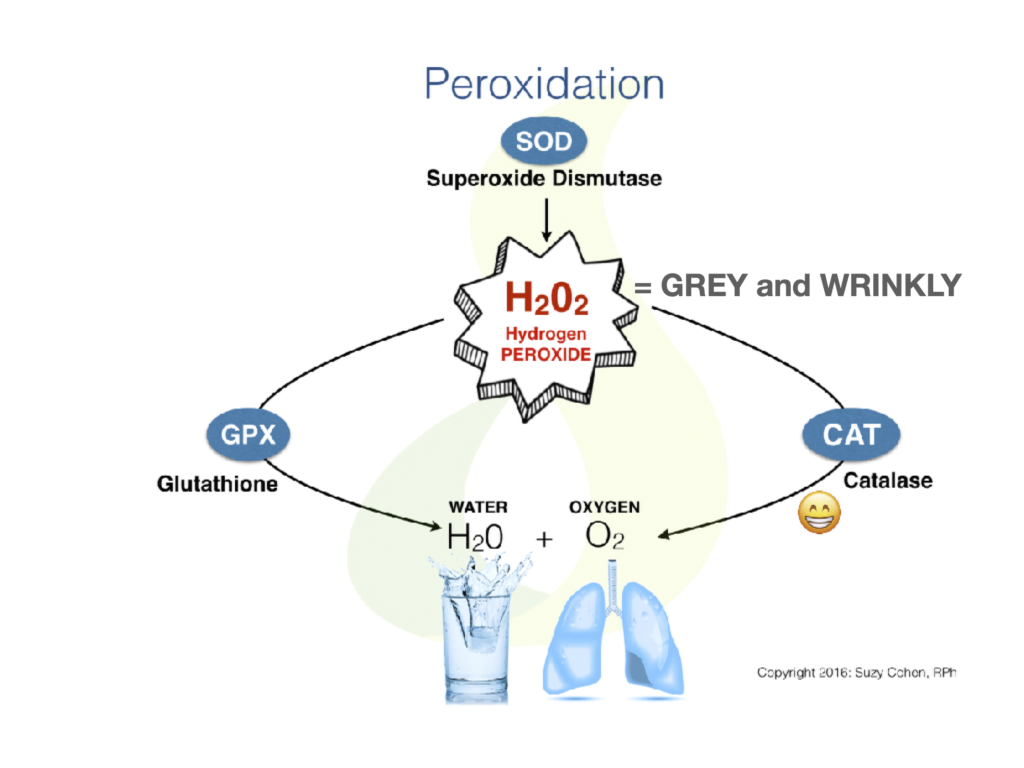
Catalase for Vitiligo?
So just by the fact that you have vitiligo says to me you are catalase deficient and if you’re catalase deficient you have high peroxide which goes hand in hand with Hashimoto’s. I posted the story of Michael at THIS site, which you can scroll to read. You’ll see his before and after pictures, he used to have Alopecia areata. If you were sitting with me having a cup of coffee and I could just be honest with you, I’d say to you, “Please don’t worry about the actual name of each of these conditions you have, and whether or not you have a third one, Hashimoto’s… but rather, focus on the ONE BIG problem which is immune dysfunction.
Your immune system needs healing and there’s one big driver of that, and it is likely something you’re eating. Once you calm down the immune system, all these different disorders will get better. But spending time and energy on each disease, by each name is going to sink you financially and emotionally.
You need to focus on the big picture. One thing is driving your immune system crazy, and it’s causing the antibodies to lodge in different areas and then you are getting labeled with this, and labeled with that, but it’s really one thing. So focus on immune health, and try not to think about what they’re labeling you with, and what’s next. Autoimmune diseases do not exist as a single disease. If you have one, you often have several. I’m going to write an article about this Cynthia, so stay tuned.
I honestly think WE ALL HAVE some degree of autoimmunity. And you can absolutely get well. Catalase may hold the key. Look into HashiScript okay, this formula may be of benefit for you, considering your immune imbalances. I think it’s worth a try. Read 15 Tips Because We All Have Some Degree of Autoimmune Disease.
Thyroid Disorders in Children
Question:
Hi there Suzy,
I have a question regarding thyroid disorders in children. I don’t see much on this topic but I have a suspicion that thyroid disorders may be at the root of many childhood anxiety disorders, behavioral disorders, learning disorders, tic disorders and or growth issues. I’d love more information on this if there is any available.
Thank you.
Manuela
Answer: Manuela there’s a lot of work done in pediatrics to try and figure out what causes all those different issues. Hyperthyroidism is definitely one condition that is associated with behavioral disorders such as hyperactivity, ADHD and agitation. The measurement of thyroid biomarkers, antibodies to Tg and TPO and TSH levels should be considered in children with learning disorders.
It could also be hypothyroidism or Hashimoto’s. But also, keep in mind that any exposure to lead, either prenatally or during childhood development is associated with many different neurocognitive impairments, including ADHD. Sometimes it’s a pathogen like a STREPTOCOCCAL INFECTION, or Lyme disease. Lyme is best tested for through the lab called Igenex. There are so many possibilities but you’re right pediatric thyroid disorders are possible, and they are rarely tested for.
Continue Antibody Testing?
Question:
Hi Suzy,
I just recently started swishing hyrdogen peroxide around in my mouth because a friend told me it helps whiten her teeth. Is this harmful to the thyroid? I have been taking Synthroid for hypothyroidism for 25 years and just recently, have started getting tested for thyroid antibodies. My TPO was a little over 200 the first time and 95 just recently, my Thyroglobulin was less than 244 both times.
Now that I know I have Hashimotos, and am starting to follow an auto-immune diet, is there any reason to continue to get antibody testing? Is it enough to just get the TSH, FT3 and RT3 and FT4 tests run in the future?
Thanks,
Lori
Answer: Hi Lori. I would stop the swishes with Hydrogen Peroxide, and use something natural like The Natural Dentist “Heathy Gums Rinse” or “Tooth & Gums Tonic” by Dental Herb Company which are made with essential oils. Also, I would continue to monitor your antibodies, twice a year, so you can track your progress and see if you’re body is responding your new autoimmune treatment plan. That said, if you feel really good then I would not bother with the antibodies except maybe once or twice a year, certainly you don’t have to do that every month or two like some doctors say.
Question:
Hi Suzy,
I’ve been diagnosed with hypothyroidism and take Nature-Throid daily. I’ve been told my issue is primarily a conversion issue between T4 and T3, but I did have low levels of TPO antibodies. At what point does this become Hashimoto’s versus hypothyroidism and would the treatments be different between the two?
Thanks,
Kim
Answer: Nature-Throid is a combination of T3 and T4 and very clean, it is frequently used for hypothyroidism. As for this “conversation,” they’re saying that your T4 isn’t converting to T3 in the tissues (peripherally) so you have all the symptoms of hypothyroidism but your TSH would be normal. Your TPO antibodies may be low if you can’t mount an effective immune response. Doctor’s don’t typically treat hypothyroidism and Hashimoto’s any differently, they give out the same medications for these conditions. Unfortunately, most physicians miss the immune piece of this.
With Hashimoto’s the immune system must be addressed, and all the free radical damage (reactive oxygen species) that harm the body. Hypothyroidism could be due to different things, for example low iodine, surgically induced or poor peripheral conversion. Hashimoto’s (which by the way drives many cases of hypothyroidism) is a full-body phenomenon and requires you to treat the immune system, to stop the self attack. I also suggest you take antioxidants, certain specific proteolytic enzymes and digestive enzymes to help with the increased intestinal permeability.
_____
Question:
I have all these symptoms you mention, and have been to every specialist under the sun only to be told I needed a mental doctor because I had mental issues. How do you know what tests to get if you are “normal.”
Traci Gaultney
Answer: That’s awful, shame on them! You haven’t been to anyone intelligent enough to test you properly. I want you to have an intelligent conversation with the next “specialist” you see so I need you to be smarter than who you are speaking with so you can fight for yourself. A complete list of tests that I recommend are listed in Thyroid Healthy, in case you have my book. There is free information at my site, and also a 1 hour video posted on YouTube. CLICK HERE.
Here are the main labs, and also USE MY SEARCH BOX for more information on this topic and labs.
Free T3: 3.5 to 4.5
TSH: 1.5 or less
TPO: Less than 10
Reverse T3: Less than 15
Ferritin: > 50
Autoimmune panel through Cyrex Labs
_____
Question:
Dear Suzy,
I enjoyed your video. I think I am in serious trouble. I have all kinds of symptoms of low thyroid. I DON’T have a thyroid and doctors can’t seem to get my dosage right. I have nails that are split from top to bottom,yet my doctor says that she doesn’t base any thyroid problem on fingernails. I gave her one of your books, “Thyroid Healthy .” I hope she reads it. This is the only endroconologist in town and she is new in town.
I have been to internist and they just take my TSH and say I am ok. But I know I am not. Finally got doctor to test my rT3 (reverse T3) after I read your book. Dr. didn’t want to test me at first, but I insisted and won out. On a scale of 1-19 . Mine is 40. That alarmed her enough to prescribe T3.
I had never heard about rT3 until I read your book. And I have been on thyroid medication for 25 years. Never once did a doctor mention rT3. So thankful for your info. So my question is , what do I take to help with my medication when I DON’T have a thyroid ?
Thanks…Ann
Answer: Hello Ann– One reason for high rT3 is heavy metals, so consider chlorophyll, chlorella or a superfood green product to help with that in the gut. I would consider an adaptogen to support adrenal health too, that will support general health and refresh your body. Something like Tulsi, Rhodiola, Ashwagandha or Shisandra. There are others, even licorice. Read about all of those and see what’s right for you. There’s some information on these if you want to watch my video, CLICK HERE.
_____
Question:
Hi Suzy,
I have a question about Graves’ disease. I have had an autoimmune issue for about 20 years now. I did at one point have hyperthyroidism and was on Tapazole, but since having my last child, my blood work has been normal. Long story short, I feel like all my symptoms could be related to Graves’ disease but, my thyroid numbers are perfectly normal. I continue to get worse as my blood work numbers stay normal.
I want to feel better and be better, but no one will help me. What can I do to get the doctor to think outside the box? What other tests can be done? I eat healthy, exercise and take many vitamins, so I am trying to do what I can to help myself.
Thank you,
Heather
Answer: You should try to get in with a Functional Medicine doctor, or maybe a holistic-trained Medical Doctor who can evaluate other things like your adrenals and cortisol levels, like your food sensitivities, and your estrogen and progesterone levels. The autoimmunity may continue despite normal levels associated with Graves’ disease. I think Cyrex lab testing for autoimmunity can help you, and also GI Effects stool test. Any doctor can order these, they may have to become a provider which is nothing more than faxing a license.
Get them both done because something is driving the discomfort. The stuff you take may just be a bandaid. I don’t want you to waste your money. In the meantime, digestive enzymes and antioxidants can help, but they are not the ultimate answer. Motherwort is an herb used for Graves’ by the way. LDN is an option too. Read my article on Low Dose Naltrexone: https://suzycohen.wpengine.com/articles/the-medicine-your-doctor-never-told-you-about-but-should-have/
_____
Question:
I read that “…several beverages commonly drunk by humans can contain H2O2 at concentrations above 100 micro-M, including green and black tea and especially instant coffee.” I make kombucha with green & black tea. Would the fermentation process help reduce the H2O2 levels? I’ve been diagnosed with hypothyroidism for over 20 years but I know in my gut that just taking my Armour Thyroid isn’t helping me. I’m overwhelmed with the all the research I’ve been doing over all those years and I’m really tired of all the things I’ve tried and not getting better. Thank you for being on ‘our side!’ Elizabeth M.
Answer: Hi Elizabeth– No, those foods don’t reduce H2O2 to my knowledge, and they are not that great for people with Hashimoto’s. I know a man who felt better in just 5 days after stopping the Kombucha when I told him to. You might consider the same. Do you have my ebook yet? It’s called “Hashi No-No’s” it will explain that kombucha may be bad for you… it’s related to the histamine production in case you didn’t get the ebook yet. The special offer is still available HERE, or you can get the ebook by clicking the link below:
_____
Question:
Thank you for email. I have been diagnosed with Hashimoto’s my antibodies were over 7000 and it was a problem just getting out of bed. I finally agreed to try Synthroid and have been taking it for a couple of years. My antibodies have dropped down to around 500 however the weight has not budged. Hope you might have some suggestions and I would really like to be medication free, or is that asking to much? I am taking 125 mg Synthroid. What is up with the depresseion, anxiety, panic attacks and headaches from having Hashimoto’s disease? Is there one way to treat all of the symptoms without going to the doctor?
Jeanice B.
Answer: No, you need a good medical doctor. I offer natural options for getting well and for getting that Synthroid to convert to T3 in my book Thyroid Healthy, it’s available here.
Among the nutrients I discuss in that book, minerals are key, especially selenium because it supports healthy antibody levels and also is known to help with Hashimoto’s. It does not interfere with Synthroid. But by no means will taking this one mineral be the cure. Have your TPO and TG antibodies measured, it’s not just about TPO, those may be fine but the TG may be swinging. Also adrenal health, there’s an entire chapter available on that in my book, and a FREE 1- hour youtube video on it.
_____
Question:
Hi Suzy
Thanks for this. I really need help too been ill years but my case is complicated.
1 question is this: After years of getting my highlights at the hairdressers, one day I had a very bad reaction to blonde hair dye in the hairdressers. As soon as she put it on my heart raced my breathing went weird and I felt like my head was going to explode!
She had to wash it off straight away and I went outside to get air. I haven’t had my blonde highlights done for 2 years as I am petrified. I am hypothyroid and have Hashimoto’s. My question is do you think my reaction to the hair dye is to do with this ‘hydrogen peroxide’ you said is in our bodies? This is fasinating as I am at the hairdresser tomorrow but not getting any colour 🙂
Thank you so much for helping us ?
Rose
Answer: Yes Rose, I think you are having some kind of allergic reaction, do not go near that again. It’s pretty clear.
____
Question:
About 8 years ago I got Thyroid Cancer, by that time they also diagnosed me with Hashimoto’s disease.
So they take out my whole thyroid, does that mean I do not have Hashimoto’s anymore, because I do not have a Thyroid.
My doctor keep me on Synthroid 112mg.
Thank you!!!!
Connie W.
Answer: Hi Connie– You are a survivor and a thriver! The Synthroid is used to replace what your thyroid used to make. Correct, you do not have Hashimoto’s anymore.
Question: Loved your videos on the effects of H2O2 (peroxide) related to thyroid health. Is there a way to increase catalase naturally without using supplements? Thank you for all you do.
Jean W.
Answer: It’s a good question. No, not really, unless you think big picture and support the health of your liver. Catalase and glutathione are made in the liver so protecting that organ protects your ability to produce those enzymes. There are some studies that suggest tocotrienols may help fight the damaging effects of hydrogen peroxide. Finally, T3 or triiodothyronine and thyroxine (T4) significantly stimulate hair follicle pigmentation so having healthy levels of thyroid hormone will affect hair color.
_____
Question:
Dear Suzy,
After reading your article on thyroid issues based around hydrogen peroxide, all makes sense and hoping your soon to be released supplement will be my answer. I have been on thyroid meds for the past 18 years with little or no success. This is frustrating me to the point of depression and frustration that the symptoms still persist, thinning hair, eyebrows, inability to lose weight, lack of energy, rarely a whole nights sleep (insomnia) Diets, (have tried ’em all)! I have noted the greens connection with goitrogens, so have been taking your Thyroid Greens powder in my shakes.
I was diagnosed with Hashimoto’s years ago and have listened every webinar available and no one has mentioned the hydrogen peroxide connection, until your latest research. But, if you do I will get to the point, with my question. When the new supplement is launched, do I continue to take my meds, (Levoxyl and Thyronine) and should I add the Thyroscript, so there would be a combination of supplements and ‘scripts? I just want so badly to have the best results with optional, functioning good health.
Cynthia H.
Answer: Hi Cynthia– After 18 years, and no help, it just makes me want to give you a big hug. I’m sorry, I really understand and I want you to hold on. One day there will be a CLICK for you, and something will shift, you’ll see. There’s so much research going on now about thyroid. Hydrogen peroxide is needed to make thyroid hormone. It’s not bad, but if it becomes elevated and excessive then it is very bad. So this may be part of what needs to happen for you. To answer your questions, my supplement ThyroScript (and/or HashiScript) would be taken along with medicine, there’s no need to stop medicine. Medicine replaces thyroid hormone.
My supplements work to support your digestion, your adrenal glands and your immune function. They also contain antioxidants designed to help break down excessive peroxide. I would recommend the HashiScript for you first, and once you’re stabilized and things turn upward for you, then you can bring in the ThyroScript if you want. It may not be necessary. Do keep up with my Thyroid Greens, that’s a superfood blend of fruits and veggies, and it won’t interfere with anything. The chlorella is amazing in and of itself.
_____
Question:
Suzy,
I went to a wellness doc who drew all suggested labs after I reported a history of Hashimoto’s and have been taking Levothyroxine for years. She said though my T-4 was normal with the Rx, I wasn’t making any T-3 so she put me on Cytomel. After being on that for a bit my blood work showed I no longer had any antibodies. So does that mean I no longer have Hashimoto’s? Most of the regular medical physicians I’ve seen since her have questioned me being on Cytomel, saying its not usually used in treating hypothyroid. Kind of frustrating and I don’t know who to believe or what kind of MD will help me treat this best.
Thanks for what you do.
Cheryl S.
Answer: Hi Cheryl– I can understand why they question you… Levothyroxine is the #1 selling thyroid medication in most regions. It is a pure T4 drug. Your T4 levels must have been in the normal range because you said your T4 “was normal with the Rx.” So I agree with your physician for prescribing the Cytomel, that is a T3 drug and it will balance your hormone levels and make you feel stronger, more energetic and healthier. T3 is the gas pedal in the body. Many people if not most do not convert the T4 drugs to T3 properly, it’s what I call “thyroid sick” in my books. So I would believe the doctor who put you on the Cytomel, she must have evaluated your T3 levels and found them to be low.
She might be seeing the big picture which is that your Levothyroxine (T4) is not converting and forming T3 properly, so she put you on it with a drug. It’s pretty simple. As for your antibodies, they never checked antibody levels for TG (thyroglobulin). They need to do that before deciding if your Hashi’s is gone. But here’s the thing, if these antibody levels are within normal range, I would shed the label of Hashimoto’s in 2 seconds! I don’t like labels and don’t like defining people by their lab work you know?! If you don’t fit the bill for the disorder, drop the disorder and celebrate. By definition if you do not have TG or TPO antibodies, you don’t have the disorder. Some will argue you with me, suggesting that your immune system might be so tanked and suppressed that you can’t make antibodies… however, that’s the time to evaluate how you feel. If you’re feeling good, drop the label.
_____
Question:
Dear Suzy,
Thank you for your work and for sharing helpful information and providing quality supplements. I am interested in your opinion on the relationship between the MTHFR genetic mutation and how both contribute to autoimmunity.
I realize that what I am about to share here is not a beautiful, double blind, research hospital study, but I also know it is not “nothing”. I personally know 24 women who, like myself, are RH-negative and we were all given RhoGam injections during pregnancy. I actually was given 4 injections in less than a year due to an ectopic pregnancy and later a healthy birth; one injection after emergency surgery for ectopic pregnancy, one during healthy pregnancy, and two at delivery because first one at delivery had a negative response from a mother in same batch. Now, 22 of the 24 women now have Hashimoto’s, myself included. Thank you again and God bless.
Allycia J.
Answer: Hi Allycia, You’ve been through so much. RhoGam contained thimerisol between 1968 and 2001, this is a type of mercury. There are lots of stories of people dealing with problems after the shot, I read a few stories of ladies developing Hashimoto’s after the shot, but these were anecdotal. The shot itself can cause immune activation and this would be lighting the fire in a person with established autoimmune disease (diagnosed or not) such as Hashimoto’s. But again, you have to weigh the risks and benefits to something like this. You made the right decision. I was able to find a study you something on your direct question of genetic mutations and autoimmunity, and MTHFR association.
Both MTHFR (methylenetetrahydrofolate reductase)and MTRR (methionine synthase reductase), are enzymes essential for DNA methylation, so it’s not just about MTHFR. If you’d like to read about MTRR, I wrote an article HERE.
Simplifying the research article published in the Clinical and Experimental Immunology (full paper available HERE) it suggests that hypomethylation due to various different polymorphisms (but not MTHFR) may cause an increase in homocysteine and caspace 3, and that this may be correlated with symptoms as well as prognosis in patients with Hashimoto’s and Graves’ disease. It also suggests that polymorphisms expressed in the MTRR gene (again, not MTHFR), observed more frequently in people with severe Hashi’s than in those with mild Hashi’s.
Due to widespread reduction in methylation, the homocysteine levels will increase caspase-3 activity and, then you get apoptosis (cells committing suicide) in the thyroid gland in people with Hashi’s (who have MTRR gene mutations). Read my article HERE. High homocysteine induces caspase-3 activity and apoptosis in various other cells but this caspase-3 is HIGHLY expressed in the thyroid of patients with Hashimoto’s.

Suzy Cohen, RPh, has been a licensed pharmacist for over 30 years, blending conventional medicine with natural approaches to help people feel better and live healthier. She is the founder of Script Essentials, a supplement company known for targeted, custom-formulated products, some with patented innovations.
With a special focus on thyroid health, functional medicine, and drug-induced nutrient depletion (what she calls “drug muggers”), Suzy is the author of several books including Thyroid Healthy, Drug Muggers, and Diabetes Without Drugs. She also writes a nationally syndicated health column and shares practical, easy-to-understand guidance with readers around the world.




