What's On This Page?
ToggleMany times, when a woman is fatigued and experiencing post-menopausal symptoms, practitioners are quick to recommend hormone replacement therapy, referred to as HRT. Sometimes the fatigue is related to hypothyroidism, or Hashimoto’s and if that’s the case for you, down below I have more information for you.
This can mitigate the symptoms of menopause, and particularly serves as a quick first-line defense against hot flashes, usually the most troubling of all menopausal symptoms. HRT is used to elevate your estrogen (and sometimes progesterone, testosterone and/or DHEA) to a higher level, akin to what you had when you were younger.
Estrogen is typically provided as a prescription called “estradiol.” You can receive prescription hormones via pills, patches, pellets, and creams. Estradiol is one of the 3 sisters of estrogen… remember, estrogen refers to a combination of estradiol, estriol and estrone.
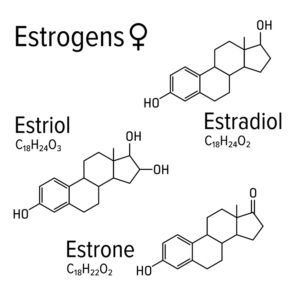
Unfortunately, many physicians prescribe the one “sister” by herself, meaning they just give you “estradiol” and not the other two estrogens. They also do not always give you progesterone with the estrogen medication.
This is a mistake in my opinion.
The estrogen prescribed all by itself, is termed “unopposed estrogen.” Despite progesterone’s far-reaching impacts on health, many doctors still wrongly assume its only job is to protect the uterus, and they don’t usually prescribe it with estrogen.
But there are receptors everywhere in your body for progesterone, so you need it whether or not you still have a uterus.
Taking estrogen and/or progesterone doesn’t always help because you might also be deficient in pregnenolone or DHEA, two hormones that are higher up on the chain. What you may not have realized until this moment is that all of your hormones start with cholesterol. Suppressing cholesterol production with medication suppresses hormone production.
It could essentially put you into mild menopause and andropause without you even realizing it!
The cholesterol is at the top of the pathway, and it goes on to form your ‘Fountain of Youth’ hormone called DHEA. Read my article on DHEA by CLICKING HERE.
The cholesterol could form either DHEA, or it could go down another pathway and form progesterone. Both DHEA and progesterone require cholesterol for their formation.
They cannot be produced without cholesterol, although that particular step is not shown in my graphic below. Take a look at what happens to progesterone. It can form one of three different hormones, cortisol, aldosterone or testosterone.
The testosterone forms estradiol thanks to an enzyme called aromatase which drives the reaction. If you want more testosterone, and less estrogen you need to take, or eat, an aromatase inhibitor.
That’s what DIM and I3C are; they are aromatase inhibitors, so they slow down the breakdown of testosterone to estrogen. That’s great for people with estrogen dominance, which often shows up as heavy periods. You may want to read my other article about Estrogen Levels Affect Guys and Gals.
So you know the content of my blog, I will now succinctly list the 8 strategies (before going over them in detail below).
- Hormone Replacement Therapy (HRT): Primarily elevates estrogen, sometimes combined with progesterone, testosterone, and/or DHEA.
- Bio-Identical Hormone Therapy: Provides hormones in forms biologically identical to what the body naturally produces, usually as customized topical creams.
- Oral Hormones: Not generally recommended due to poor survival through stomach acid and potential side effects.
- Injections: Provide direct delivery into the bloodstream but carry risks of incorrect dosing and potential difficulty in adjusting quickly.
- Pellets (Implants): Offer steady hormone dosing, but adjusting dosage is challenging once implanted.
- Topical Hormone Creams: Easier to adjust dosing, offering flexibility to stop or modify dosage quickly if side effects occur.
- Aromatase Inhibitors (e.g., DIM, I3C): Help reduce conversion of testosterone to estrogen, useful for estrogen dominance issues.
- Adrenal Support: Incorporating adrenal health strategies, like stress management and adaptogens, to complement hormone therapies.
The Importance of Supporting the Adrenals During Menopause
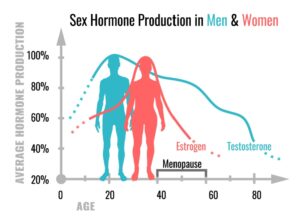
When considering hormone replacement therapy (HRT), it’s easy to focus solely on estrogen, progesterone, and testosterone, but another critical factor to address is adrenal health. Your adrenal glands play a key role in producing hormones like cortisol, DHEA, and even a small amount of estrogen and progesterone after menopause. As ovarian production of these hormones declines, your adrenals pick up some of the slack, making them a vital part of the hormonal balance puzzle.
Chronic stress, poor diet, and lack of sleep can overburden your adrenal glands, causing what’s commonly referred to as “adrenal fatigue.” This can exacerbate menopausal symptoms like fatigue, brain fog, and sleep disturbances. Therefore, it’s important to support your adrenals through lifestyle adjustments such as managing stress, eating a nutrient-rich diet, and considering supplements like adaptogenic herbs (ie ashwagandha, or rhodiola) to promote adrenal balance.
Incorporating adrenal support can make a significant difference in how well you respond to HRT or bio-identical hormone therapy. It helps create a more stable foundation for hormone production, ensuring that your body is better equipped to manage the changes brought on by menopause. Make sure to discuss adrenal health with your healthcare provider when considering any hormone treatment plan.
 The Trouble with Some Synthetic Hormones
The Trouble with Some Synthetic Hormones
Certain HRT medications come with an increased risk of breast and uterine cancer as well as the small, but potential, risk of heart attack, deep vein thrombosis, and stroke.
Another issue is with estradiol itself. This is a hormone that’s naturally made by men and women. It is also the name of a hormone replacement drug. In other words, you can buy estradiol at the pharmacy by that name, or many other brand names. My concern is not the drug, but rather the dose.
Oftentimes, the prescription version is much, much higher than you’d typically make. Too much of this highly active estrogen can lead to cell and tissue proliferation (ie cancer or tumor growth). The fact that estrogen can fuel hormone-dependent cancers, is well known.
Hypothyroidism and Estrogen
Results from a scientific paper I read in the Journal of Thyroid Research are very compelling and point to estrogen’s ability to regulate genes which control cell growth and cell cycle progression of thyroid cells. That’s not good. It means that excessive estradiol could be contributing (at least potentially) to the development of thyroid cancer or thyroid hyperplasia.
I want to make sure I’m informing you, not scaring you. Too much estradiol is bad for your thyroid and may contribute to thyroid cell hyperplasia or what might become thyroid cancer.
You can read: Role of Estrogen in Thyroid Function and Growth Regulation by CLICKING HERE.
HRT medicines are potent drug muggers and capable of suppressing nearly every mineral in the body as well as your B vitamins.
Because of this drug-mugging effect, take synthetic HRT long enough, and you’ll have even worse fatigue, depression, hypothyroidism, confusion, memory lapses, anxiety, insomnia and weight gain.
CLICK HERE to purchase a copy of my book Drug Muggers.
You can choose bio-identical hormone therapy if traditional HRT doesn’t improve your post-menopausal symptoms. Doing so provides your body with estrogen and progesterone in forms that are biologically identical to what was naturally produced in your youth. That means you experience more of the benefits, and fewer side effects. These therapies are usually created in compounding pharmacies as topical creams, and the dose is customized for you. The dose is determined by the amount that you make, as well as your response.
I don’t like oral hormones generally speaking, I’ve never tried them personally, but I know they won’t easily survive your stomach acid unless you take synthetic ones (which I don’t believe in). You will do better with topically applied hormones I feel.
Injections? Who here wants to go near needles?! It feels unnatural to me and I also feel like it’s harder to gauge your dose. Incorrectly dosed estrogen increases the risk that a woman will develop endometrial cancer (cancer of womb). The longer a woman uses an estrogen, the greater the risk she encounters. This goes for oral contraceptives and HRT. So the idea of injecting estrogen leaves me feeling uneasy.
What if the dose is too high? The acute side effects will be difficult to mitigate quickly because the hormone went straight into your blood stream.
Other Hormone Strategies
Some people use pellets which are implanted beneath the skin. There are certain advantages to those, for example, steady dosing (less peaks and troughs), and they can be made as bio-identical. It’s really up to you. My opinion is (and this IS my opinion blog), that it’s harder to quickly adjust your dose because you can’t easily get those out!
You see, hormones are part of a spider web but it’s true. You can’t pull one part of the web without impacting the rest. Plus, hormones take a long time to get to your doctor, and also for those hormones to clear the body, usually 3 to 6 weeks. If you don’t do well on an implant (or injection) it’s hard to get that out of you. Sometimes the side effects of improper hormones (however they are provided to you) include spotting, irritability, headaches, weight gain, breast tenderness, acne, and insomnia. If you’re experiencing that, every minute matters.
Whereas with a topically applied hormone cream, you simply stop applying it! Or you squeeze out a tiny bit, instead of the recommended dose. It’s pretty easy!
Dosing Hormone Strategy
It’s a trial and error thing, so when you start with bio-identical hormones, you should ask the Compounding Pharmacy if you can purchase just a week or two at a time, so you can test it and gauge your symptoms and side effects. If it causes you to feel unwell somehow… like you get agitated, drowsy, sleepless, dizzy or something else, then your physician can call in something different and you can buy another couple of weeks at a time.
Doing it this way allows you to be sure that adjustments to your hormone prescription can be dialed in perfectly for your body, and then you can go ahead and buy a 90-day supply. Take the DUTCH Complete Test that I offer, and you’ll get a free ebook to help you with all of this.
Oftentimes, the bio-identical hormones used in the cream include some or all of the following: DHEA, testosterone, estriol, estrone, estradiol and progesterone. Estriol is hardly ever mentioned but it’s a fun fact that the placenta produces this estrogen in large amounts during pregnancy. Find a physician in your city that specializes in reading labs and prescribing hormones, rather than just asking your General Practitioner for a one-size-fits-all pill.

Suzy Cohen, RPh, has been a licensed pharmacist for over 30 years, blending conventional medicine with natural approaches to help people feel better and live healthier. She is the founder of Script Essentials, a supplement company known for targeted, custom-formulated products, some with patented innovations.
With a special focus on thyroid health, functional medicine, and drug-induced nutrient depletion (what she calls “drug muggers”), Suzy is the author of several books including Thyroid Healthy, Drug Muggers, and Diabetes Without Drugs. She also writes a nationally syndicated health column and shares practical, easy-to-understand guidance with readers around the world.



