What's On This Page?
ToggleRheumatoid arthritis or RA is an autoimmune condition that leads to joint damage. As a person goes through the process of getting diagnosed, various tests are done. A complete workup, physical exam and medical history are important because the blood tests have shortcomings.
Rheumatoid arthritis is inflammatory, painful and usually progressive. But there are many interventions today that can keep you strong and healthy for a long time, despite having the diagnosis.
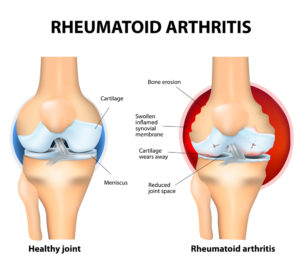
Two Popular Tests for Rheumatoid Arthritis
1. Rheumatoid Factor
Measuring levels of Rheumatoid Factor (RF) is important, but despite the name, it is non-specific to RA meaning that other disorders can cause a positive result. People with diabetes, bacterial endocarditis, vaccinations, a history of transfusion, or cancer (even getting older) can increase RF levels.
Furthermore, about 20% of people who have RA will have a perfectly normal RF level! To make it even more perplexing, a person can have total control of their rheumatoid arthritis and feel really good, but their RF level will remain high! So you can see that it’s unreliable all by itself. What makes this test super confusing is that negative levels do not ensure that you’re free of rheumatoid arthritis. So current standard of practice is to add another test in the workup which I will discuss next.
2. The Anti-CCP Antibody Test
This is a slightly more specific test for RA (rheumatoid arthritis), but it can also be helpful in finding other autoimmune disorders like lupus and Sjogren’s syndrome.. I’ll call this the “CCP test” for short, but the lab isn’t measuring CCP levels, they’re actually measuring your antibodies to the CCP (Anti-cyclic Citrullinated Peptides).
These CCP peptides are commonly produced if you have RA and they attack the joints. Any result up to 20 u/mL is negative. Just like RF levels, having high antibodies to CCP (a high level) doesn’t necessarily mean you have rheumatoid arthritis, it could be predictive.
And there’s one more scenario. If both your anti-CCP and RF tests are negative, your doctor may STILL diagnose you with rheumatoid arthritis based on your symptoms and clinical presentation.
Natural Strategies for Rheumatoid Arthritis Pain
-
Vitamin D is Helpful
There was a significant correlation found between vitamin D and rheumatoid. This STUDY determined that people with reduced vitamin D levels have higher anti-CCP levels. This suggests that treatment with vitamin D could help people with RA. The authors of this study concluded, “Serum 25-OH-D level was negatively correlated to anti-CCP antibody level and disease activity, which implied the therapeutic role of serum 25-OH-D in rheumatoid arthritis.”
If you’re vitamin D levels are low, a good strategy is to figure out why. That’s very important. Are you deficient in vitamin D because of any of the following?
6 Reasons You Might Be Low in Vitamin D
- You don’t get enough sun.
- Your kidney or liver function isn’t up to par. See note below.
- You have parathyroid disease.
- You have Lyme disease (diagnosed or not).
- You have eczema or asthma.
- You have a VDR (Vitamin D Receptor) gene polymorphism
2. Improving liver function may help with rheumatoid arthritis
Your liver health determines how well you activate the sunlight-derived vitamin D. And vitamin D is critical for rheumatoid patients. For that matter, many studies have proven that low D increases autoimmunity for other diseases, not just rheumatoid. Give your liver a break by avoiding alcohol, nicotine, weed, junk food, and refined sweets.
I mentioned it above in my list, regarding #2 where I stated, “Your kidney or liver function isn’t up to par.”
I wanted to expand on this because many people believe that once you expose yourself to sunlight, you get a sufficient amount of vitamin D. This is not the case for most people.
The cutaneous absorption of D does not automatically mean that the precursor form of D gets converted to the active hormone called calcitriol, which is the type of D that does all the work in the body. Metabolically speaking, the liver converts vitamin D to 25OHD. Then your kidneys convert this newly formed 25OHD to 1,25(OH)2D and 24,25(OH)2D. See it’s more complicated than going into a tanning bed, or to the park to get some ‘sun.’ There is more about the details of conversion in this paper from the National Library of Medicine.
In order to convert vitamin D to a biologically active form, various other minerals are essential in each cell. These include phosphorus, calcium, and zinc. Proper healthy amounts of parathyroid hormone (PTH) must also be present.
Symptoms of Rheumatoid Arthritis
Rheumatoid arthritis affects each person differently, and the speed at which it causes problems also varies. Generally speaking, RA will cause painful swelling to the joint cavity. over time, the presence of inflammatory cytokines will lead to bone erosion and joint deformity. Below I list some of the symptoms that occur within the joints, as well as those that occur outside the joints, termed “extra-articular.” Not all of these symptoms occur in each person because RA manifests differently.
- Tender, hot or warm inflamed joints
- Joint stiffness that is more evident upon arising, or after periods of inactivity
- Fatigue
- Occasional fever and/or loss of appetite
- Mood instability
- Dryness of the eye and/or iritis
- Lumps under the skin “rheumatoid nodules”
- Scarring within the lung
- Plaque build-up in the arteries
- Dry mouth if the salivary glands become involved
- Neuropathy (pins and needles)
- Changes in BONE MARROW
- Vasculitis may occur in chronic cases
- Fingernail changes, ridges, yellow color, thickening of the nail bed, and splintering
3. Collagen supplementation may help but it must be the right type.
There have been some positive benefits seen anecdotally with collagen supplementation. It makes sense because that’s where the attack is targeted. The problem is that people take the wrong type of collagen for their cartilage.
The joints, ligaments, tendons, and cartilage can only take a very specific type of collagen, notably Type II. You can avoid a mistake by learning more. Read the longer version of my article, which you can receive by email after signing up for my free health newsletter at suzycohen.com.
Collagen’s role in the management of rheumatoid arthritis has been questioned in the past, due to this being one of the tissues attacked by the body’s own immune system. That’s why there is not a solid body of evidence that agrees about collagen supplementation and rheumatoid.
There have been some studies, but most of them are flawed in some way. Anecdotal evidence and support are abundant, and it makes logical sense to replenish what is being destroyed in order to keep a balance of new collagen, vs that which has been compromised and destroyed.
There was a 2017 paper I found that showed oral collagen supplementation could improve stiffness and inflamed painful joints, but not to the extent that drugs help. People say it helps, and that’s good enough for me to suggest a trial for you. But you would want to make sure it’s Type II collagen, not Type I or III (which is great for skin, hair, and nails.)
There are more than 15 types of collagen that have been identified.
The human body is comprised mainly of type I, II, or III.
Type II collagen is what a person with rheumatoid arthritis symptoms wants. This is a type of collagen that supplement sellers offer for joint health, and it is the type of collagen extracted from chicken bones.
More substantial research is needed to see if collagen peptides can keep RA from progressing, but certainly, we can say Type II collagen supports joint health, cartilage, tendons, and ligaments.* There’s this STUDY from 1993 that talks about it. This is another positive STUDY regarding Type II collagen (which goes by many brand names, including Kollagen® which is one of the featured ingredients in my custom formula Joint Script).
When combined with natural TNF blockers, cytokines are managed. This can make a remarkable difference in terms of comfort. You can learn more about how to achieve this HERE.
Taking collagen supplements can help symptomatically but it doesn’t cure anything. The immune system is attacking itself, and the collagen won’t fix that. The best solution is to figure out if there is an infection, food antigen, vitamin D deficiency, or parathyroid disorder that is causing the problem. There are many issues that lead to the development of rheumatoid arthritis, and many are not listed here so talk to a qualified physician.
4. TNF Alpha Inhibitors and DMARDs plus Natural Supplements
The use of TNF-blocking medications for rheumatoid arthritis is common. Inflixamab is a common drug used for this purpose, which you may have heard of, Remicade.® Adalimumab is another, it goes by Humira.® These drugs are game changers for some people, so I’m not going to knock them. They are right for some folks, and not right for others based upon your individual sensitivity to side effects, prior medical history, genetics and length of time with disease.
The Difference Between Rheumatoid Arthritis and Osteoarthritis
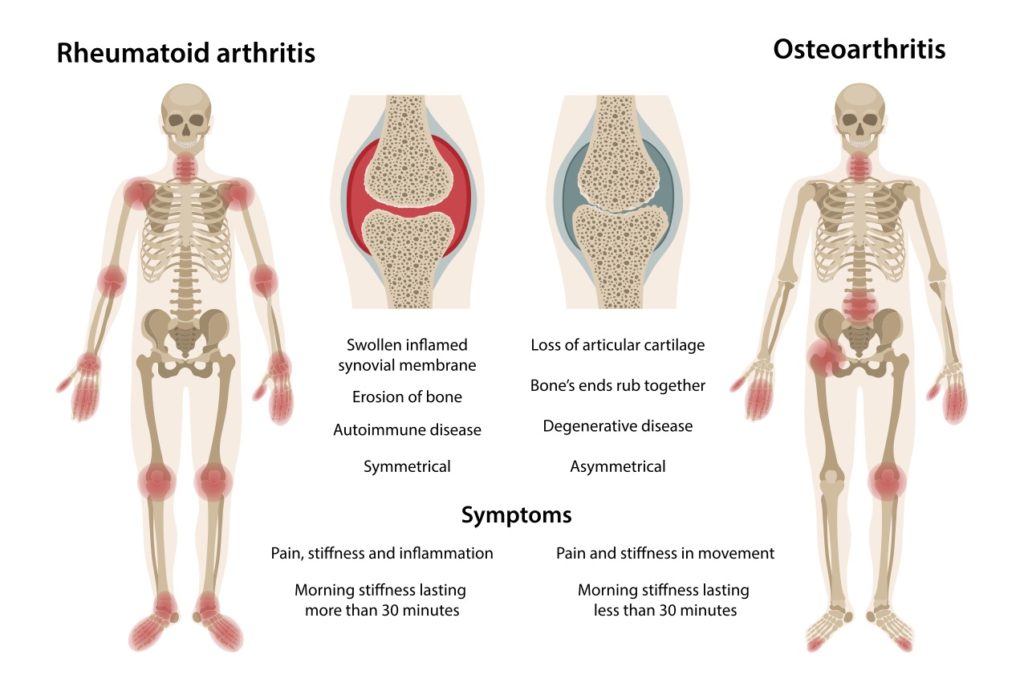
You should know that when you chronically block TNF, you suppress the number of inflammatory chemicals that are released. Further, when you block TNF, you also suppress the immune system, the entire immune system! So while the self-attack slows and symptoms begin to abate, you become more susceptible to otherwise simple infections like a cold or flu, or cold sore, etc. Cancer risk goes up with long-term use. The FDA issued a BLACK BOX WARNING which you can review at your leisure.
Then there are the biologics that are sometimes prescribed along with the TNF inhibitor drugs. These are also called DMARDs (disease-modifying anti-rheumatic drugs). Popular medications in this category include methotrexate, sulfasalazine, hydroxychloroquine, and leflunomide. They are not the same as NSAIDs which work differently but also help with rheumatoid pain.
But sometimes side effects make these medications intolerable, and if that’s the case for you, there are two very potent, natural TNF blockers. You can discuss these natural remedies with your physician. There are others not listed here as well.
1. Black Seed Oil
2. EGCG supplementation (found in green tea)
TNF (Tumor Necrosis Factor) rises in the body and increases inflammation and joint destruction. You can reduce TNF naturally by improving your blood sugar levels, doing yoga/tai chi, falling in love, or going on a keto diet!
If you are looking for a natural “DMARD” there are all kinds of natural remedies, but they’re weaker. Remember, a DMARD is just a drug that blocks TNF, but you can do that with Mother Nature’s arsenal (to some degree). Natural TNF-blocking supplements include fish oil, EGCG, rooibos tea, black seed oil, curcumin, PQQ, and hops.
5. Doing yoga or Tai Chi
These types of exercise and movements help stretch your muscles and keep you in good shape, not to mention reduce inflammatory cytokines. Stretching with warmth and humidity (for example, a warm yoga class) may cause fewer injuries. Be careful and always exercise to your own level and capabilities.
What About Foods?
You may be interested in the ebook I’ve written: The 9 Best Foods for Arthritis.
If you have a moment, read THIS ARTICLE on Bartonella, a co-infection of Lyme that is associated with rheumatoid arthritis.
In Closing
Having a complex disorder like rheumatoid arthritis is a challenge. The two main tests for rheumatoid are RF and anti- CCP antibodies. These tests are not conclusive in terms of specificity. Elevated levels of CCP shown on a blood test may be reduced by vitamin D supplementation for some people. Treatment of rheumatoid arthritis is based on the severity of discomfort.
Collagen is useful if it is the right type. Where Type I and III are fantastic for beauty needs, it is Type II that works on the joints. Taking 5 or even 10 different types of collagen is useless, yet supplement sellers offer products to naive consumers. The human body only has an abundance of Type I, II, and III collagen, and whatever else you take beyond that might spawn a low-grade autoimmune reaction in you because those other types of collagen peptides are foreign to the human makeup.
Type II collagen supplementation has not been proven to reverse rheumatoid arthritis but may offer mild symptomatic relief for some people. Be careful about the type of collagen product you purchase, many contain more ingredients than you need that can trigger autoimmune reactions in the body.
As humans, we only recognize Types I, II, and III for the most part. I sell collagen, so I’ve studied it extensively, and I know that joints, tendons, and cartilage respond only to Type II peptides. Read your label, or learn more HERE. The advice to reduce stress, and to stretch and eat right is certainly wise, but they don’t hold a candle to reducing antibody levels of CCP, and inhibiting TNF alpha.
Many people suffering from the pain of arthritis find comfort and relief from stiffness by taking a warm bath or getting into a steam room. The moist heat is relaxing to muscles and relieves some degree of rigidity.

Suzy Cohen, RPh, has been a licensed pharmacist for over 30 years, blending conventional medicine with natural approaches to help people feel better and live healthier. She is the founder of Script Essentials, a supplement company known for targeted, custom-formulated products, some with patented innovations.
With a special focus on thyroid health, functional medicine, and drug-induced nutrient depletion (what she calls “drug muggers”), Suzy is the author of several books including Thyroid Healthy, Drug Muggers, and Diabetes Without Drugs. She also writes a nationally syndicated health column and shares practical, easy-to-understand guidance with readers around the world.





