What's On This Page?
ToggleThe thyroid gland is shaped like a butterfly and it regulates your body temperature, how fast you burn fat, and your energy levels. Most people with hypothyroidism do not even know they have the condition because they are not doing the correct labs, or misinterpreting the results.
There is a good correlation between the thyroid gland’s functioning and your total levels of cholesterol and LDL. A rule of thumb is that the lower your thyroid hormone, the more lipid (cholesterol and triglyceride) abnormalities you have. Even borderline thyroid problems are associated with lipid abnormalities. We are not 100% sure why that is, however, some researchers theorize that there is impaired LDL receptor functioning.
The Problem is that People with Hypothyroidism Have a Higher Heart Attack Risk
Well for one, most people with hypothyroidism do not even know they have the condition because they are not doing the correct labs, or they are doing the labs but misinterpreting the data, or perhaps they’re asymptomatic.
So the problem is that subclinical hypothyroidism may increase heart attack risk. The term “subclinical hypothyroidism” means that it’s very early in the disease process, and that the levels are not dangerously low, and that the level of TSH might be slightly above the normal range.
Anyone who has been diagnosed with cholesterol (lipid) abnormalities should have a complete thyroid hormone profile conducted. Cholesterol drugs may affect your thyroid gland, and reduce thyroid levels possibly causing or contributing to hypothyroidism! The reason this could happen is through the drug-nutrient depletion effect, what I call the “drug mugging” effect. Statins block production of natural CoQ10, Vitamin D, and selenium-containing proteins (think glutathione). Side effects associated with statin drugs very much mimic the picture of a deficiency of all of these nutrients. You cannot make adequate thyroid hormone without selenium by the way!
If you take a statin type of medication, I urge you to take high-quality versions of these nutrients and eat a healthy well-balanced diet. Doing so will mitigate some of the side effects of the statin. Speaking of side effects, muscle problems are top of the list. By the way, statins don’t vacuum cholesterol out of your arteries, they just reduce the amount you produce with every pill.
Statins are far more likely to cause muscle pain, cramps and skeletal muscle damage if you already have hypothyroidism (diagnosed or not). So you can see why it’s important to have a thyroid profile done at least once a year and more often if you take a statin.
If you’re a practitioner, then please always consider your patient’s thyroid status before you prescribe a statin drug or any lipid-lowering medication. If you’re a patient trying to make sense of this, then ask for a complete thyroid profile. It’s a blood test. Today’s laws actually permit you, the patient, to visit some qualifying labs and get this type of test all done by yourself.
The clinical pearl I want to relay today is that taking a statin if you have hypothyroidism could be harmful because there is a situation called thyroid-induced myopathy, and it will be exacerbated by the statins. The reason is that statins are well-known to induce myopathies galore! It’s probably their #1 side effect!
Another Connection Between Statins and Thyroid Hormone
The next situation worth noting – and this isn’t too well known- but cholesterol drugs may affect your thyroid gland, and reduce levels of thyroxine which either cause or contribute to hypothyroidism. One reason this happens is via the drug-nutrient depletion effect, what I call the “drug mugging” effect. This leads me to the number one prescribed cholesterol medication in the world, known chemically as “HMG-CoA reductase inhibitors.” Now you know why we just call them “statins.”
Anyone who has been diagnosed with cholesterol (lipid) abnormalities should have a complete thyroid hormone profile conducted. You can self-order tests if you’d like at many labs today, or you can go through my practitioner link for DIRECT LABS and buy the test there: Scroll down and click on this test “Thyroid Panel Complete-August Test of the Month”
You can of course, request the test from a local physician at your next check up.
Statins don’t vacuum cholesterol out of your arteries, they just reduce the amount you produce moving forward. As soon as you start taking them, your body stops making as much cholesterol as it used to, and cholesterol forms the backbone for testosterone, estrogen and brain neurotransmitters.
A Little More Side Effects…
Statins are potent drug muggers of many nutrients, in particular CoQ10. I was among the first health bloggers to ever alert consumers about this effect back in 1998, and I took a lot of flack for it! I had to defend that statement with research over and over to physicians that thought I was the new quack in town. Today, virtually every doctor knows this as a fact.
Always keep in mind that statins negatively affect your ability to absorb your thyroid hormone medication, and produce thyroid hormone so it will be contributing, if not causing thyroid disease in some people.
The Thyroid Gland Keeps You Focused and Fit
The thyroid gland is one of your most important glands because it keeps you warm, happy, energetic, fit, and focused. Without adequate hormone production, you will not be able to metabolize fats. So you won’t be able to properly mobilize and break down your cholesterol (or other fatty acids in the liver). At its core, thyroid hormone is a fat burner and cholesterol is fat.
So it might be bad because as your thyroid hormone declines, you will gain weight, feel tired, deal with poor concentration and focus, and you might have bouts of anxiety and depression. Plus, you might feel cold all the time. One more thing, you could experience some hair loss, either on top of your head or eyelash/brow loss.
Muscle Problems
You might get muscle problems from taking statins and that would make existing muscle problems terribly worse! Statins are far more likely to cause muscle pain, cramps, and skeletal muscle damage if you have hypothyroidism (diagnosed or not). Rhabdomyolysis is the most feared and potentially fatal complication of taking these types of medications. Atrophy of muscles is another rare possibility.
So you can see why it’s important to have a thyroid profile done at least once a year and more often if you take a statin. Your muscles are important and once damage occurs, it can become very uncomfortable. In fact, it may not even be traced to a medication you started 2 or 3 years ago! If the topic of restless legs and muscle problems is of interest to you, CLICK HERE to read my article, Akathisias Make You Want to Jump Out of Your Skin. And you might like this article too, 5 Benefits of Using a Weighted Blanket.
Statins are known to cause myopathy, and this risk and the level of discomfort is compounded by you having hypothyroidism. Doctors sometimes miss this, it’s easy to miss… but it’s a fact that many patients have overlapping symptoms from statin-induced myopathy and hypothyroidism.
If it’s missed, they’ll give you a pill for this and a pill for that! For example, a pill for pain, and another for muscle relaxation… a pill to sleep and another for restless legs. And with all those, you’re going to soon need a reflux drug to soothe your stomach, which causes about a dozen major drug nutrient depletions!
Magnesium is so potently reduced by PPI drugs that it could trigger cardiac arrhythmias, that’s why there’s a black box warning on those drugs! This warning was issued in 2011, so I hope you know about it. If not, READ HERE.
These drugs are sold over-the-counter, so you may not even realize that. Plus, with all the new weakness, and back pain or leg pain, it’s likely you’ll get sent out for expensive MRI or CT scans “just to make sure it’s not something serious.” In most cases, the results of that will be “unremarkable” because there is no finding on a scan when the trouble stems from the drug mugging effect! You can’t see CoQ10, selenium, magnesium, potassium, Vitamin D or any other depletion on an MRI!!! But these depletions can cause very serious and real human suffering.
What About Thyroid-Induced Muscle Pain
A simple test might determine if muscle weakness, pain and tenderness is associated with hypothyroidism. The test to ask for is “creatine kinase.” Hypothyroid patients with muscle pain and musculoskeletal symptoms usually have elevated serum creatine kinase (CK) levels in their blood work.
The treatment of this condition (hypothyroidism) with some thyroid hormone medication will usually alleviate symptoms of myopathy and might even help with the lipid/cholesterol ratios! But if you’re not tested for CK levels or hypothyroidism, it will get missed and then your statin drug will make these muscle problems even worse.
You can see why treating hypothyroidism can address several issues all at once, and yet the test is something that some of you still have to fight for. It’s head-scratching to me when I receive letters like this from MaryJo:
“It took my doctor almost 2 years of pleading and phone calls, and I took him your book but he said it was not my problem. I finally got the FULL thyroid test you recommended and I’m so glad about this!!!! He reluctantly gave me some medicine Immediately after the first week on Armour and I felt better than I have in the last 8 years!! It’s been about 2 months right now and I’ve lost 10 pounds too. Cannot say enough about you right now I only wish I hadn’t waited so long.”
Blood tests for these things should be the #1 thing you do before you opt-in for statin drugs, and then subsequent medications to treat side effects such as muscle relaxers, analgesics, and sleeping pills. A good endocrinologist will know all this.
If you do start medication for thyroid, be aware that there are significant interactions with popular items such as diary (because of the calcium content) as well as iron supplements like “ferrous sulfate.” You need to separate your thyroid medication (Levothyroxine) from these by 4 hours.
List of Interactions Between Thyroid Medicine and Other Medications:
- Proton pump inhibitors
- Acid blockers
- Estrogen-containing drugs
- Sucralfate
- Calcium carbonate (ie Bone supplements or Tums®)
- Carbamazepine or phenytoin
- Statins (they may reduce thyroid medication activity)
- DMARDS (ie hydroxychloroquine, cyclophosphamide, methotrexate, sulfasalazine, leflunomide and others)
- Corticosteroids for arthritis, allergies and more (Prednisone, Hydrocortisone, Dexamethasone and others)
What should you do if you take these other medications with thyroid?
Adjustments to your medication can be made if you don’t enjoy the benefits within a couple of weeks, but just make sure you are closely monitored and doing your initial tests so dosage adjustments can be made. Keep in mind that the TSH (Thyroid Stimulating Hormone) is one test that evaluates the basic function of the gland. It does not give you details regarding levels. To check for that, have your Free T4 and T3 evaluated as well as Total T4 and T3. Your endocrinologist can review this with you, or you can turn to page 52 of my Thyroid Healthy book to see recommended ranges for all of this.
Aside from statins lowering thyroid levels, another drug that can do that is Lithium. If you are taking 300mg or more per day, this can impact the functional activity of your thyroid gland.
What if you’re taking both thyroid medicine AND a statin…
Since many doctors prescribe both statins and thyroid medicine, it’s important to know if that’s okay. It’s actually been studied using simvastatin. Levels of TSH and Free T4 were evaluated during the course of treatment in a STUDY entitled “The Effects of Simvastatin on the Serum Concentrations of Thyroid Stimulating Hormone and Free Thyroxine in Hypothyroidism.”
Forty-one patients taking 20mg of simvastatin were evaluated and their levels of Free T4 (FT4) and TSH were studied.
The scientists concluded with, “…the findings of the present study suggest that there may not be any significant interaction between simvastatin and levothyroxine.”
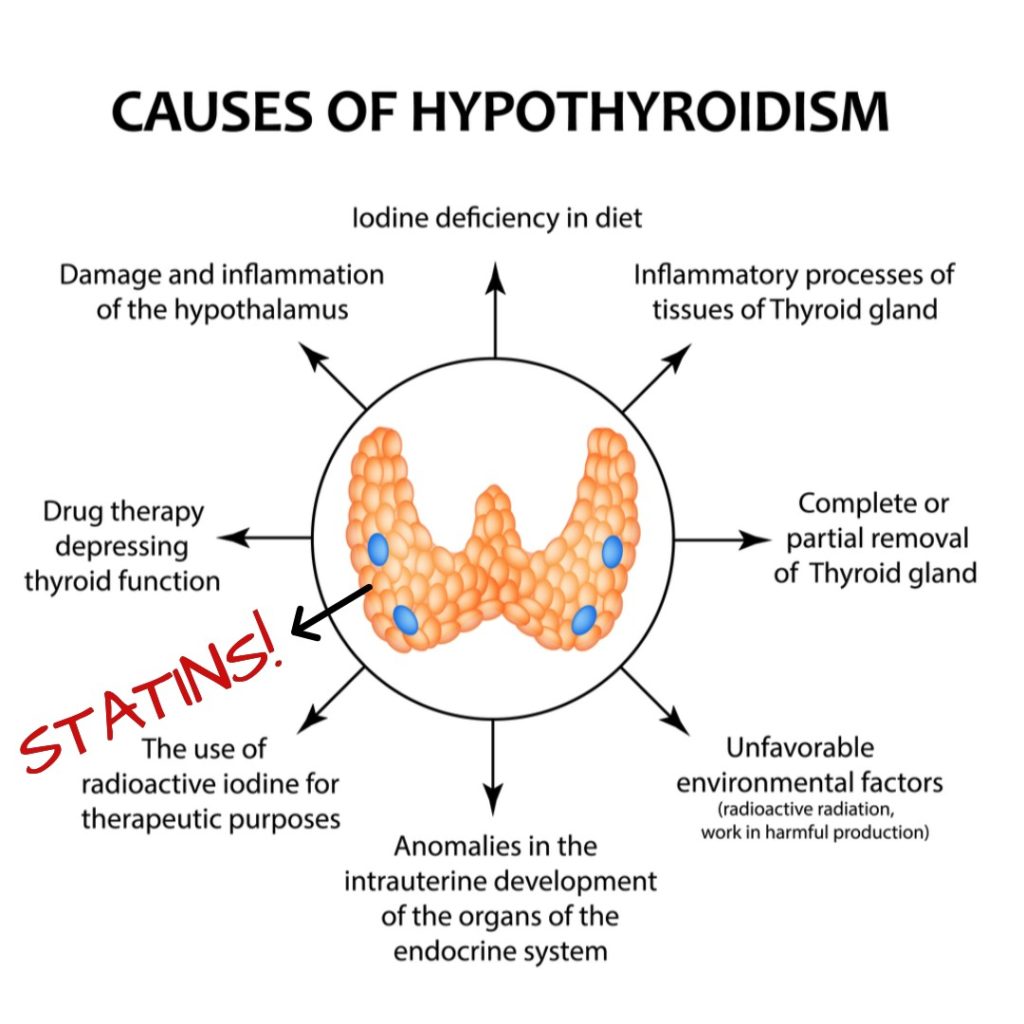
What about Graves’ disease or hyperthyroidism?
The opposite effect occurs meaning that elevated thyroid hormone could lead to a reduction in total cholesterol.
In conclusion, if you’re a practitioner, then please always consider the patient’s thyroid status before you order statin prescriptions or any lipid-lowering medication. If you’re a patient, you have every right to ask your doctor for a full thyroid profile (or panel), in fact, you can self-order this test if you desire. That is allowed now as outlined in my article, You Can Order Your Own Blood Work and Lab Tests.
CLICK HERE to find out how.
Before I close, I want to describe the details of a very important case study about a man who experienced hypothyroidism-induced problems with cholesterol or triglycerides.
He lacked the typical symptoms of low thyroid. See above for the list of symptoms.
This led to a misdiagnosis and the inappropriate use of a statin. That resulted in severe statin-induced myopathies. This highlights a few important issues:
- You may not have clear symptoms of hypothyroidism! Some people have woefully bad labs, and yet they’re nearly asymptomatic!
- The case STUDY I’m referring to was for a 55-year-old man who had a TSH level higher than 100 mU/L which is ridiculously high. The relationship is inverse, so a level like this means he was ridiculously low in thyroid hormone! Very hypothyroid.
- Using a statin in someone who has hypothyroidism could be harmful if you’re not careful because the thyroid-induced myopathy will be exacerbated by the statins, which are known to induce myopathies. It’s like their #1 side effect pretty much!
No one is 100% sure of why there is thyroid-induced myopathy, however, there are theories circulating about “glycogenolysis” or impaired mitochondrial oxidation. Regardless, the use of a drug that has adverse effects on muscles could be detrimental on people who already have pre-existing muscle problems such as those with hypothyroidism (diagnosed or not, symptomatic or not).
Generally speaking, the higher the dose of statins, the more muscle pain, and myopathy occurs. It’s dose-dependent. It’s not just statins, by the way. Other lipid-reducing medications, such as fibrates (ie clofibrate, gemfibrozil, or fenofibrate) and even ezetimibe (Zetia®) an inhibitor of intestinal cholesterol absorption, can also induce myopathy.
Also, before starting your statin medication, get a baseline “creatine kinase” level. You can monitor this throughout your therapy to check the status of your muscle health. Although I have to say, you can probably feel it too! Most people on these drugs know well the muscle cramps, weakness, ashiness, back pain and spasms! But a CK level is objective, and important that’s why I’m recommending it.
According to this case STUDY “Further, if a patient’s dyslipidemia gets worse without apparent cause or he or she develops SIM unexpectedly, hypothyroidism should be considered.”
Statin therapy is much safer and more effective when you have normal thyroid levels, and this is the main point I’d like to make. If you are hypothyroid, and/or you have muscle pain already then these types of drugs should be used with tremendous caution, under doctor’s supervision, at the very lowest dose, and only if all else fails.
I want to point one thing out. Some of you don’t respond to lipid-lowering medications. There could be a reason and you should know it before you raise your statin dosage over and over. In closing, if you find yourself resistant to statins (meaning your cholesterol ratios remain high during statin therapy), it could be due to you having hypothyroidism and dyslipidemia related to low thyroid will not respond well to statins, no matter how high the dose.
Should you stop your statin?
This is between you and your doctor. I’m not one so I am not allowed to weigh in on this. As a pharmacist, I can tell you that there are pros and cons to every medication. It’s what we call the risk-to-benefit ratio.
You can make many medications more tolerable and safer for yourself by restoring what the drug mugger stole. By that I mean, by restoring the depleted nutrients. If you’re not sure what your medication is ‘stealing’ from your body, you can refer to my book “Drug Muggers” available by CLICKING HERE. You can also use my search box on this site because I’ve written about the impact of many popular drugs and all of those articles are archived here for public reference.

Suzy Cohen, RPh, has been a licensed pharmacist for over 30 years, blending conventional medicine with natural approaches to help people feel better and live healthier. She is the founder of Script Essentials, a supplement company known for targeted, custom-formulated products, some with patented innovations.
With a special focus on thyroid health, functional medicine, and drug-induced nutrient depletion (what she calls “drug muggers”), Suzy is the author of several books including Thyroid Healthy, Drug Muggers, and Diabetes Without Drugs. She also writes a nationally syndicated health column and shares practical, easy-to-understand guidance with readers around the world.


