What's On This Page?
ToggleDysgeusia is an intriguing phenomenon that can significantly impact our culinary experiences and the way we “taste” foods and supplements. It manifests as an alteration in taste perception, causing even your favorite foods to lose their familiar appeal. Sweet and salty delicacies may inexplicably taste bland, while other foods can adopt a metallic or bitter character.
What if every food you ate tasted about the same?
How about if everything was bland?
What if you had this metallic taste in your mouth?
What would you do? It seems an impossible situation, so frustrating and awful. Today, I’ll help you figure out what the cause is, and what you can do about it.
This condition of dysgeusia, often accompanied by a diminished appetite and weight loss (though not cachexia), can be perplexing and frustrating. It can lead to apathy, mild depression, weight loss, and more! If the topic of unintended weight loss is of interest, I wrote another informative ARTICLE about that.
Imagine savoring a bite of buttery mashed potatoes, only for it to evoke the sensation of rusty nails on your palate. While this analogy may be unsettling, it underscores the profound impact of taste distortion.
What about when something as plain as water tastes bad?! Notably, when water tastes metallic, it might indicate an underlying issue like iron overload. Dysgeusia is not a mere hallucination but rather a genuine taste distortion that your mind struggles to comprehend. You may perceive yogurt as rancid, even though those around you taste it for all of its deliciousness.

Even dietary supplements that are in capsules intended to be flavor-neutral, may take on unpleasant tastes for individuals with dysgeusia. This was brought to my attention recently by someone who perceived a bad taste from neutral capsules. No one else could taste them the same way. Dysgeusia can lead a person to believe and insist that the capsules (the supplement) is rotten or rancid. It can be upsetting to all involved and there isn’t a real solution.
Capsules that are supposed to be non-offensive can be perceived as tasting metallic, rancid, or bitter. If you doubt this assertion, have someone else sample the capsules to validate your experience. Dysgeusia is not a conspiracy, it is a real phenomenon with complex underlying causes.
Causes of Dysgeusia
Numerous factors contribute to the development of dysgeusia, including various medical conditions. During the COVID-19 pandemic, many people lost their sense of smell and taste, it was fairly common and millions of people have reported this adverse event. Luckily, most people had both of these sensory misperceptions return to normalcy.
But still, it made post-recovery dining awful for weeks if not months. Some people still suffer from this lingering symptom, if only intermittently. A deficiency of zinc may be partly to blame. I wrote another article about 6 Critical Reasons You Need Zinc.
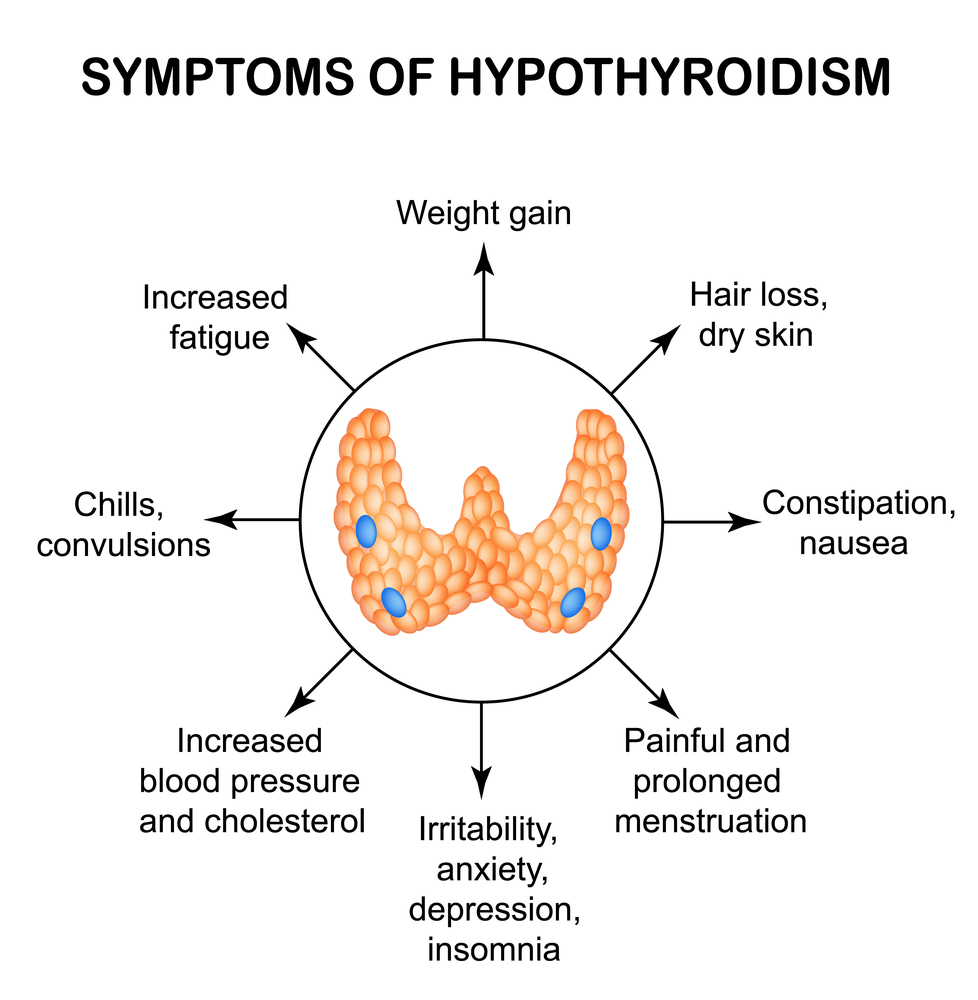
Hypothyroidism and Dysgeusia
Additionally, hypothyroidism, a condition characterized by an underactive thyroid, can wreak havoc on your taste buds, leading to the perception of sweet and salty foods as “oddly” flavored. Thankfully, the good news is that dysgeusia tends to be temporary in this case too, and repairs itself naturally once your thyroid hormone levels are brought back to normal.
Zinc Deficiency in Dysgeusia
Recent studies have also suggested a link between zinc deficiency and dysgeusia. Zinc is a crucial micronutrient involved in taste (and smell) perception. A deficiency in this essential element can disrupt the normal functioning of taste receptors, resulting in distorted taste perceptions.
Therefore, it is essential to ensure an adequate intake of zinc-rich foods in your diet to support optimal taste sensation or supplement with a high-quality form of zinc that’s gentle on the stomach. Visit my VITAMIN SHOP for something like that.
Medications and Taste Perception
The bitter truth is that many medications can play tricks on your taste buds and cause you to experience the problem. I would say that ACE inhibitors, antibiotics, and chemotherapy drugs top the list. Drug-induced dysgeusia is very common, more common than most people think.
Compounded with taking a drug listed here, and having had COVID in the past and/or hypothyroidism you might very well be experiencing weird or awful taste sensations on things that people find quite palatable or neutral. Here are a dozen different medication categories that are on my ‘watch list’ for causing dysgeusia. Do you take any of these?
- Thyroid Medication: People who take “Levothyroxine” or the popular brand Synthroid® may experience hypogeusia, or full-on dysgeusia. This could be happening due to the drug itself causing it (which I would say is very very rare), or reduced levels of zinc which often go hand-in-hand with hypothyroidism.Most likely, the problem is just from the phenomenon of being hypothyroid! We don’t have to complicate it. It just so happens that people with low T3 activity perceive foods and supplements differently (badly) than those with normal thyroid activity. Same with smell, it’s reduced or they have phantosmia.
- Statins: Cholesterol-lowering medications like atorvastatin and simvastatin have been reported to cause taste changes, including a metallic or bitter taste. Not all statins cause taste distortions though.
- Antipsychotics: Some antipsychotic drugs, such as haloperidol and chlorpromazine, may lead to taste alterations, including a bitter or unusual taste sensation. Risperidone is another interesting psychiatric drug that can cause dysgeusia (as well as indigestion), but the irony is that the drug usually leads to weight gain, whereas most drugs that cause dysgeusia lead to weight loss.
- Antibiotics: Beyond metronidazole and tetracycline, other antibiotics like clarithromycin and erythromycin have been linked to changes in taste, including a metallic taste. The antifungal griseofulvin could be classified under this heading as a potential offender.
- ACE Inhibitors: Apart from affecting blood pressure, ACE inhibitors like lisinopril can sometimes lead to taste disturbances, such as altered taste perception. It can happen within 90 days of starting a drug (if it’s going to happen). Luckily, upon discontinuation, taste returns to normal.
- Anti-seizure Medications: Medications like topiramate and phenytoin used for seizure control can cause taste changes, often described as a metallic or carbonated taste. Here’s a PAPER.
- Antidepressants: Tricyclic antidepressants, such as amitriptyline, lithium for bipolar, as well as some SSRIs like sertraline may be associated with taste alterations. I use the word “may” with caution because there are studies to show sertraline can do the opposite and help. Like in this CASE. And this case where mirtazapine helped another PATIENT. What we do know is that antidepressants can cause changes in taste sensations, and blunt bitter tastes a little bit, but each person responds differently to a medication so while some people on antidepressants get dysgeusia, others do not, and might even be helped by the drugs. I’m on the fence about it but including the category for your own educational purposes.
- Antiarrhythmics: Certain medications used to manage irregular heart rhythms, like amiodarone, have been linked to taste disturbances.

- Migraine Medications: Some drugs prescribed for migraine prevention, such as valproate or topiramate (Topamax®), have been reported to cause taste changes.
- Calcium Channel Blockers: Medications like nifedipine, amlodipine, verapamil and more are used to treat high blood pressure and angina, may lead to taste disturbances, including altered taste perception.
- Immunosuppressants: Drugs used to suppress the immune system, like mycophenolate mofetil (CellCept®), cyclosporine or tacrolimus can occasionally cause taste disturbances.
- Chemotherapy Drugs: There are medications that are used to treat various cancers in the body such as breast cancer, ovarian cancer, melanoma, Hodgkin’s lymphoma, Multiple Myeloma, leukemia, lung cancer, testicular or prostate, colorectal cancer and more.
I’m going to list these medications now because they are all potential reasons for the development of dysgeusia. Some of these drugs are also used for rheumatoid arthritis, psoriasis or other autoimmune conditions. Since these medications are administered under the guidance of oncologists or rheumatologists, speak to them about how to offset the dysgeusia should it occur. It doesn’t happen in everyone:
Cyclophosphamide
Dacarbazine
Doxorubicin
Fluorouracil
Methotrexate
Cisplatin
Paclitaxel
Vincristine
NOTE ⚠️ It’s important to note that while these medications can sometimes lead to dysgeusia, not everyone who takes them will experience taste disturbances that’s what makes it so difficult to pin the blame on your medication. What I mean by that is what if you took amlodipine for the past 8 years and only now developed dysgeusia? I would guess the sudden taste distortion was not due to the medication, but perhaps to some other more recent change in your lifestyle, or health.
That said, if you suspect that a medication is affecting your sense of taste, it’s advisable to consult with your healthcare provider. They can assess your situation and potentially adjust your treatment plan if needed.
Navigating Taste Changes: A Guide to Making it All Better!
If you’ve experienced moments when your favorite dish suddenly tastes like an alien creation, fear not, I’ve got some savvy tips to help you cope with dysgeusia like a pro.
- Embrace the Aromas: Choose foods that now smell and taste good, even if they’re not your usual go-to’s. Sometimes, your senses just crave something different, just keep experimenting.
- Banish Cooking Odors: If you’re sensitive to smell (my mom is!) use an exhaust fan, consider grilling outdoors, or grab some pre-cooked options. Cold or room-temperature foods like sandwiches are less aromatic, making them a solid choice.
- Chill Out: Cold or frozen foods can be your taste buds’ best pals. Things like a smoothie taste better than their hot counterparts. But, a quick note: if you’re on certain chemotherapy drugs (for example oxaliplatin which is known by the brand Eloxatin®, steer clear of cold foods and cold temperatures – this drug can make a person cold-sensitive termed “cold dysesthesia.”
- Go Plastic, Bamboo or Silicone: I do my best to recycle and keep our environment clean, but in some cases, you have to use plastic, bamboo or silicone. The metal forks and other utensils might be adding to the problem a teeny bit. Switching your utensils helps a bit in reducing metallic taste sensations, at least anecdotally.
- Flavor Saviors: Try hard candies with strong flavors, these can be game-changers. Something flavored with peppermint, licorice, lemon, or orange can offset or mask bitter or metallic tastes, making every bite more enjoyable.
- Red Meat Alternatives: I love a good steak but for some people with dysgeusia, it may leave you with a metallic taste in your mouth. No worries, opt for tofu, tempeh, chicken, eggs, fish, peanut butter, beans, or dairy products for your protein source.
- Get Saucy: Marinate your meats in fruit juices, sweet wines or vinegar, salad dressings, or other tasty sauces. It’ll add a burst of flavor to your dishes that might be okay for you. Just experiment.
- Spice Things Up: Don’t be shy with herbs, spices, sugar, lemon, or sauces. They can transform a bland meal into a culinary masterpiece!
- Timing Matters: Consider the clock when eating around chemotherapy. Wait 1 to 2 hours before and up to 3 hours after your session to prevent food aversions caused by nausea and vomiting. In some cases, you might have to wait longer. Speak to your oncologist about this problem because there are medications they can give you to offset the nausea (things like Zofran®).
- Rinse and Refresh: Before meals and at bedtime, rinse your mouth with a salt and baking soda solution (about ½ teaspoon each in 1 cup of warm water). It might just stop those unpleasant tastes in their tracks.
- Oral Care Matters: Keep that mouth squeaky clean with regular brushing and daily flossing. A clean and healthy mouth can work wonders for your taste buds. Gum disease and undiagnosed tooth/gum infections can cause bad breath and a bad taste in your mouth.
- Zinc Supplements: Talk to your doctor about zinc supplements. Chelated ZINC is my recommendation because it’s easier on the tummy. These may improve taste for some folks, especially those that are post-COVID. But of course, be smart and always consult with a healthcare pro before adding any dietary supplements, especially during active cancer treatment.
- Explore Marijuana: Don’t hesitate to discuss medications like Marinol® (delta-9-tetrahydrocannabinol (THC)) which is a drug from the pharmacy, or natural Marijuana which is now decriminalized in many states. Either one of these along with Megestrol acetate can be ordered (or prescribed) by your cancer team. These options might just give your taste buds a boost, and improve appetite too. They could be useful if cachexia is also involved.
Summary
It’s crucial to understand that dysgeusia is a sensory adventure, not a permanent flavor makeover. This isn’t going to persist for the rest of your life, at least not for most people. Knowing that it’s likely temporary can help alleviate some anxiety associated with altered taste perceptions.
Remember, taste changes are part of the journey, and you’re not alone. With these tips I’ve shared in your culinary toolbox, you’ll navigate the world of flavors with more ease. One of the big things is to maintain oral hygiene. And if you think you have drug-induced dysgeusia make sure to speak to your doctor for an alternative drug.
I know this is difficult for many of you reading this. Be sure to experiment with different flavors and textures to find what works best for you. This is such an individual experience that I can’t even begin to figure out what is right for you. But I do know that certain tastes can help counteract the strange ones.
By understanding some of the underlying causes, such as zinc deficiency, COVID infections, hypothyroidism, and possible drug-induced situations, you can navigate the challenges with a bit more confidence and resilience. That’s my hope and if you like this article, please forward it to a friend or post it on social media.

Suzy Cohen, RPh, has been a licensed pharmacist for over 30 years, blending conventional medicine with natural approaches to help people feel better and live healthier. She is the founder of Script Essentials, a supplement company known for targeted, custom-formulated products, some with patented innovations.
With a special focus on thyroid health, functional medicine, and drug-induced nutrient depletion (what she calls “drug muggers”), Suzy is the author of several books including Thyroid Healthy, Drug Muggers, and Diabetes Without Drugs. She also writes a nationally syndicated health column and shares practical, easy-to-understand guidance with readers around the world.


