What's On This Page?
ToggleToday, I’ll tell you about a metabolic pathway called mTOT. It may prove useful for people with various medical conditions, including Parkinson’s. It has to do with dopamine.
Parkinson’s disease, as you may know, is a progressive disorder affecting movement which causes tremors of the hands, arms, legs, jaw and elsewhere. The condition slows movements, and causes a sensation of rigidity and stiffness of the limbs and trunk. Balance can be impacted too.
A related condition, Lewy Body Disease (LBD), may look very similar to Parkinson’s but doesn’t usually present with tremors. Cognitive fluctuations are hallmarks of both disorders, depending on the stage of the condition.
By “cognitive fluctuations” I am referring to rapid changes in daytime alertness, staring spells, changes in attention and arousal, and more. These fluctuations may change from minute to minute, hour to hour, or day to day, making both diseases unpredictable and scary for patients and the people who love them.

There is debate amongst practitioners about differentiating between various senile dementia disorders based upon how rapidly these cognitive fluctuations occur. So they may have a hard time telling Alzheimer’s, Parkinson’s and LBD patients apart.
Parkinson’s and LBD
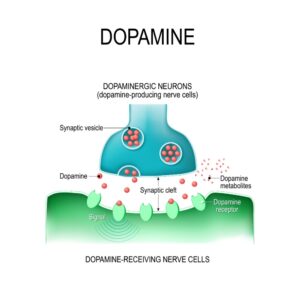
One thing Parkinson’s and LBD have in common is an issue with the neurotransmitter called dopamine, abbreviated as DA. There’s a malfunction associated with either the production of dopamine or the transport of this “passion hormone” across the synapse… or maybe suppressed “receptor sensitivity” meaning the DA (dopamine) is there but it doesn’t get “hugged” into the cell.
This is known as post-synaptic D2 receptor down-regulation. It can happen to people who do not have Parkinson’s, for example, those afflicted by withdrawal symptoms from hydrocodone, or people who took methylphenidate for childhood ADHD.
3 Genes Tied to Parkinson’s
For those of you interested in gene SNPs (genetic polymorphisms), here are the genes that break DA down (check your 23andme reports):
MAOa and MAOb = Monoamine Oxidase
COMT = Catechol-O-Methyl-Transferase
ALDH = Aldehyde Dehydrogenase
These 3 genes encode for enzymes that break down DA. If you don’t break it down, it can build up causing hedonism, hyperactivity, insomnia, mania, delusions and strong compulsions (to drink, have sex, gamble, etc.). This is NOT the case with people who have

Symptoms
Parkinson’s-like symptoms, in fact it’s quite the opposite. Low dopamine results in symptoms more along the lines of depression, apathy and postural problems, as well as all the other classic signs of low DA. I am only telling you about the HIGH symptoms of DA because the medications used to treat Parkinson’s and LBD may cause you (or your loved one) to swing too high.
Dopamine is the typical target of conventional medications used to treat Parkinson’s so I want you to be aware.
When SPECHT studies were conducted in kids on ADHD stimulant drugs, researchers concluded that their D2 (dopamine) receptors were negatively impacted.
They had a maximum of 20% functioning ability, as published in Neuropediatrics in 2003. I’ve had my eye on some research suggesting that either thiamine (vitamin B1), CDP choline or coleus forkohlii could upregulate the dopamine receptors, but I don’t have enough information yet to draw a firm conclusion.
Dopaminergic treatment may cause weight loss in people, which means you may want to take 15 minutes to read my other article on this important topic: Tackling Unintended Weight Loss: 14 Ways To Manage Cachexia.
Diabetes Medication and mTOT
What I have to tell you today is rather exciting! It’s about a diabetes drug that’s in Phase 3 studies (MSDC-0160), at the time of this writing, so it’s not named yet.
The emerging research suggests its role in Parkinson’s could be profound. It’s not due to balancing blood sugar, it’s because this diabetes agent improves mitochondrial function. Your mitochondria are the organelles that produce energy for you. They help you make ATP.
So this diabetes drug belongs to the category of “Mitochondrial Target of Thiazolidinediones” modulators (mTOT for short). These drugs make your body more sensitive to insulin. They are insulin sensitizers.
But forget insulin for a minute… the benefit of mTOT drugs is really about energy. If you can improve mitochondrial function in brain cells, you then restore the cells’ ability to convert basic nutrients into energy.
Consequently, the cells’ ability to handle potentially harmful proteins is normalized, which leads to reduced inflammation and reduced death and dysfunction of the neurons.
Since MSDC-0160 has undergone Phase II clinical trials, we know it has been compared to pioglitazone over three months. The drug showed promise by reducing plasma glucose and eliciting similar beneficial effects as pioglitazone but without too many undesirable side effects . It’s not available yet.
As for other mTOT drugs, they are in development but nothing is available for purchase at the time of this writing (March 2024). Soon though… soon.
When I worked in Florida nursing homes for 7 years, I saw a lot of this and at that time there were very few tools to use. We had levodopa, a drug from the 70’s that’s still used today, but ramping up dopamine isn’t the cure, and the side effects are concerning.
This research is intriguing, although to keep it in perspective, it was conducted in mice and there’s no human research yet. We are also not sure what the side effects will be. So the excitement is that here we have a drug intended for type 2 diabetes, that could address the underlying cause of Parkinson’s. There is hope!
mTOT Diabetes Drugs
These mTOT diabetes drugs will soon become viable alternatives to Actos and Avandia for people who can’t tolerate those or are worried about side effects. The mTOTs target the mitochondria, of which we have trillions, and we need to keep them happy! They produce energy.
These types of drugs can do that, and so you might say they paint with a broad paintbrush. The trial confirms other solid research about mitochondrial dysfunction as one of the contributing -and possibly causative – factors in Parkinson’s.
Microbiome Connection
Your gut microbiome matters in every aspect of your health, so please consider supplementing with probiotics. There is a direct connection between the microbiome and Parkinson’s.
Various other studies have shown that your gut microbiome is almost always impaired if you have Parkinson’s and that you can develop constipation and other GI problems several years before the onset of the classic Parkinson’s-associated motor problems.
I recommend taking a high-quality probiotic when you are healthy, and stay on the lookout for these GI symptoms… because early intervention can make a big difference in the progression of disease.
Related Articles

Suzy Cohen, RPh, has been a licensed pharmacist for over 30 years, blending conventional medicine with natural approaches to help people feel better and live healthier. She is the founder of Script Essentials, a supplement company known for targeted, custom-formulated products, some with patented innovations.
With a special focus on thyroid health, functional medicine, and drug-induced nutrient depletion (what she calls “drug muggers”), Suzy is the author of several books including Thyroid Healthy, Drug Muggers, and Diabetes Without Drugs. She also writes a nationally syndicated health column and shares practical, easy-to-understand guidance with readers around the world.



